Introduction
Many patients suffering from joint distension feel overwhelmed and desperate for relief, especially when faced with conditions like frozen shoulder. By mastering hydrodilatation, a minimally invasive technique that injects fluid into the joint space, healthcare professionals can offer significant relief and restore mobility to those burdened by pain. But with the right approach, there’s hope for a brighter, pain-free future.
What strategies can professionals employ to ensure a successful outcome and navigate potential setbacks in joint distension?
Understand Joint Distension: Definition and Importance
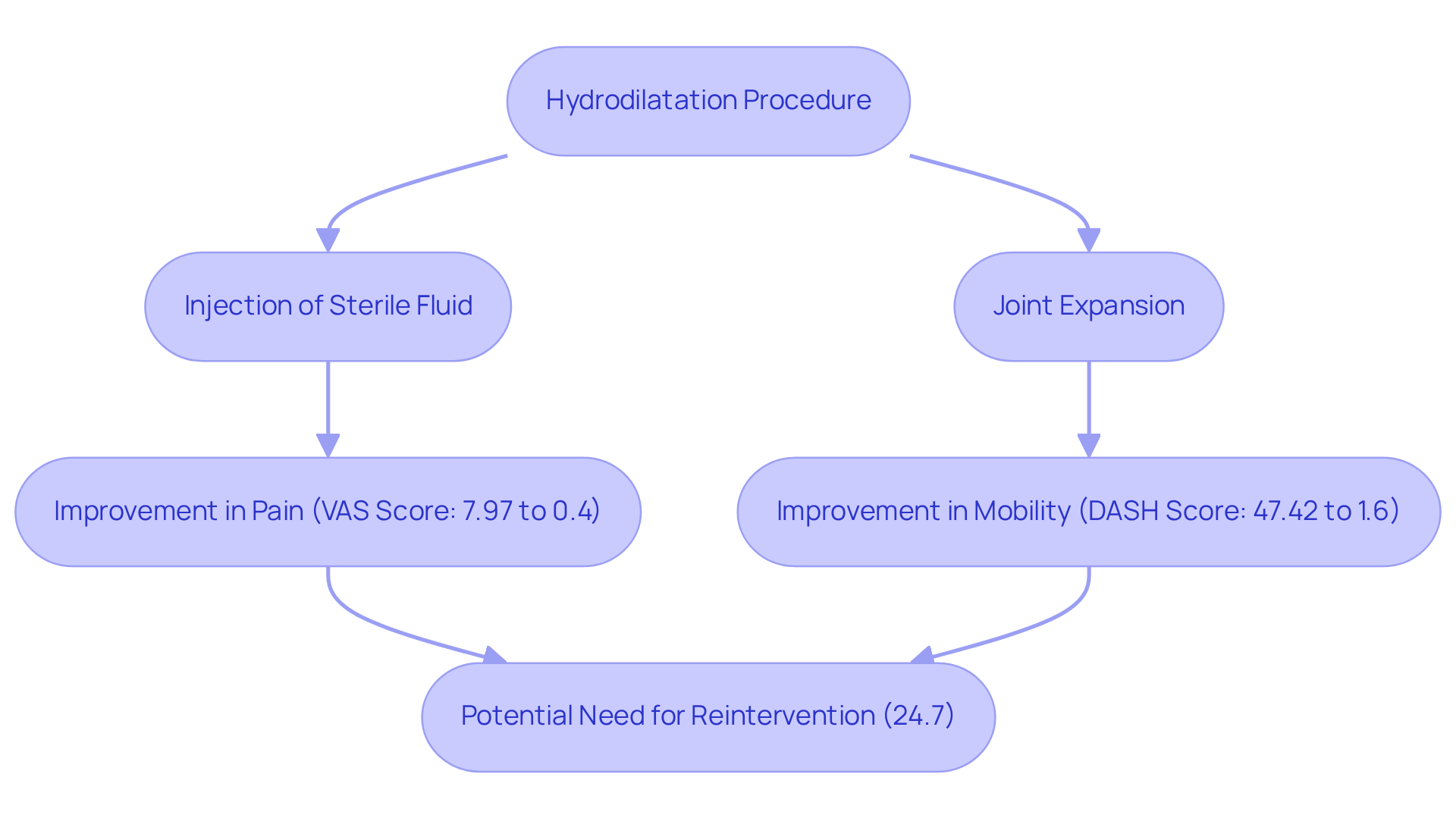
For many, the struggle with frozen shoulder feels like a never-ending battle, leaving them in pain and unable to enjoy life fully. Hydrodilatation offers a glimmer of hope. This minimally invasive technique involves injecting sterile fluid into the joint space, helping to expand it and relieve the stiffness that can be so debilitating. Patients with adhesive capsulitis often find themselves frustrated, longing for the days when simple movements didn’t come with discomfort.
Imagine the relief when research shows that hydrodistension can significantly improve your ability to move without pain. Studies reveal a remarkable reduction in pain, with the mean Visual Analog Scale (VAS) score dropping from 7.97 to 0.4 over two years. Additionally, the mean Disabilities of the Arm, Shoulder, and Hand (DASH) score improved from 47.42 to 1.6, showcasing the procedure’s effectiveness in restoring mobility and functionality.
Countless individuals have shared their stories of triumph after hydrodilatation, reclaiming their lives and passions. Many express joy at regaining their range of motion and experiencing less discomfort, allowing them to return to daily activities and physical pursuits. While a cohort study indicated that about 24.7% of individuals needed reintervention after hydrodistension, the initial relief and enhanced limb function reported by many is a testament to the procedure’s potential.
By understanding the mechanics and benefits of joint distension, healthcare providers can better assess its relevance for their patients, ultimately leading to improved outcomes in joint health and mobility. Understanding the power of hydrodilatation could be the key to unlocking a life free from pain and full of movement.
Prepare for Joint Distension: Assessments and Evaluations
Before embarking on the journey of joint distension, it’s crucial to understand the unique narrative that each patient contributes.
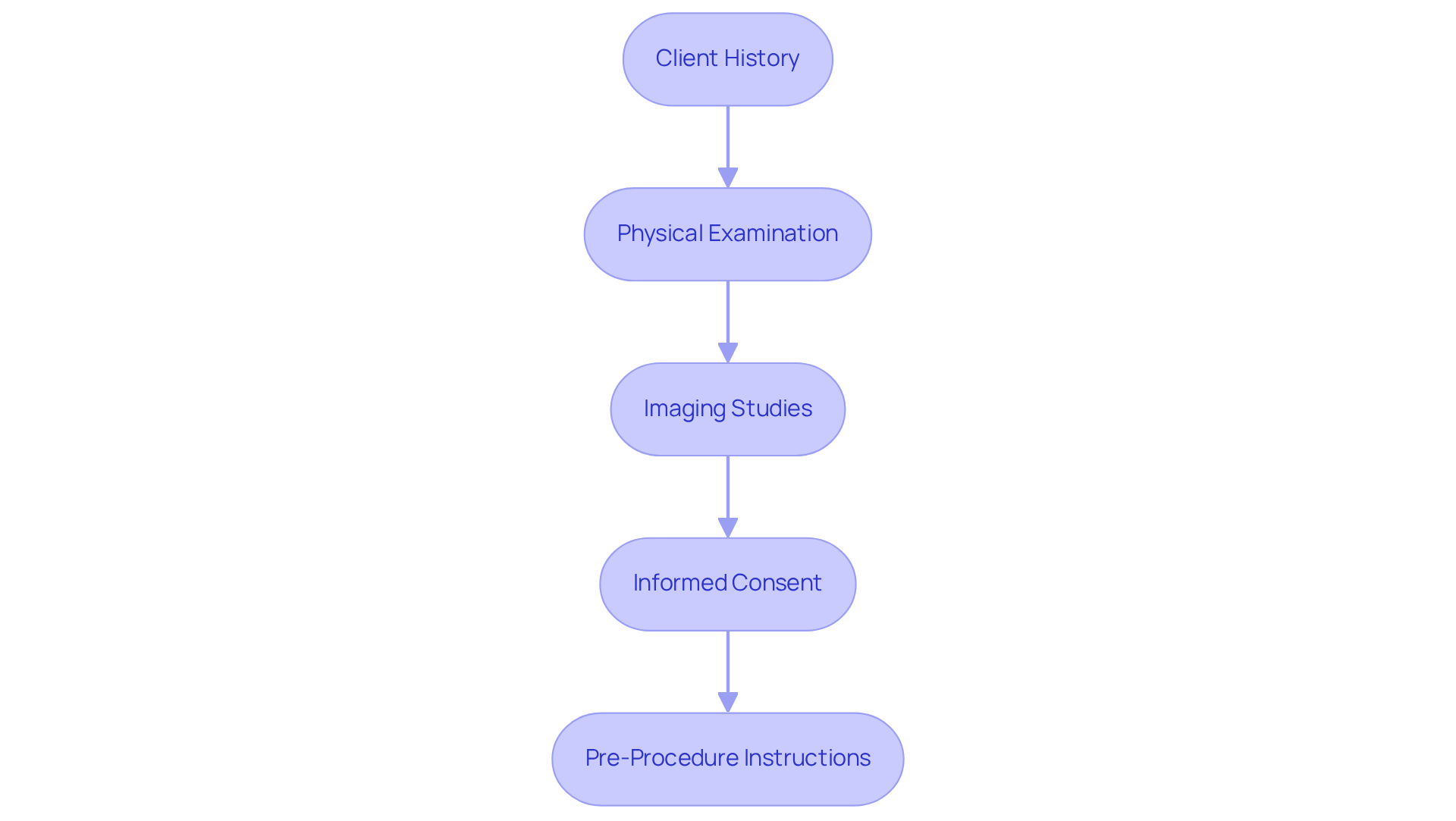
- Client History: Collecting comprehensive information about an individual’s medical background is vital. This includes past joint injuries, surgeries, and current symptoms. For instance, those with a history of adhesive capsulitis may require tailored management strategies due to a higher risk of recurrence, particularly in patients with diabetes. By truly understanding each patient’s history, we can tailor our approach to ensure their safety and enhance the effectiveness of their treatment.
- Physical Examination: A thorough physical examination of the affected area is essential. We assess range of motion, pain levels, and any signs of inflammation or swelling. This step is crucial for determining the severity of the condition and planning the appropriate intervention. At RegenCore, we focus on personalized regenerative treatments that harness the body’s natural healing abilities, helping patients recover from inflammation and injury with care and compassion.
- Imaging Studies: Reviewing existing imaging studies, such as X-rays or MRIs, helps us assess the condition of the joint. If necessary, we may order new imaging to confirm the diagnosis and evaluate the extent of any adhesions or damage. Imaging plays a vital role in understanding each patient’s unique condition, guiding us to choose the best path forward for their healing journey.
- Informed Consent: It’s important to discuss the process with the individual, explaining the benefits, risks, and anticipated results. Ensuring that the individual understands and consents to the procedure fosters trust and helps our patients feel prepared and supported every step of the way.
- Pre-Procedure Instructions: Providing pre-procedure guidelines, including any necessary fasting or medication adjustments, is crucial for preparing patients for the injection. Proper preparation can minimize complications and improve the likelihood of a successful outcome.
By adhering to these preparatory measures, healthcare professionals can guarantee that the patient is sufficiently evaluated and prepared for the joint distension process, ultimately leading to enhanced patient results. Incorporating case studies, such as those demonstrating significant improvements in pain and functionality after following these steps, including the partial regeneration of the human hip via autologous bone marrow nucleated cell transfer, reinforces the effectiveness of the procedures discussed. By taking these steps, we not only prepare for a procedure but also pave the way for healing and renewed hope for our patients.
Execute Joint Distension: Step-by-Step Procedure
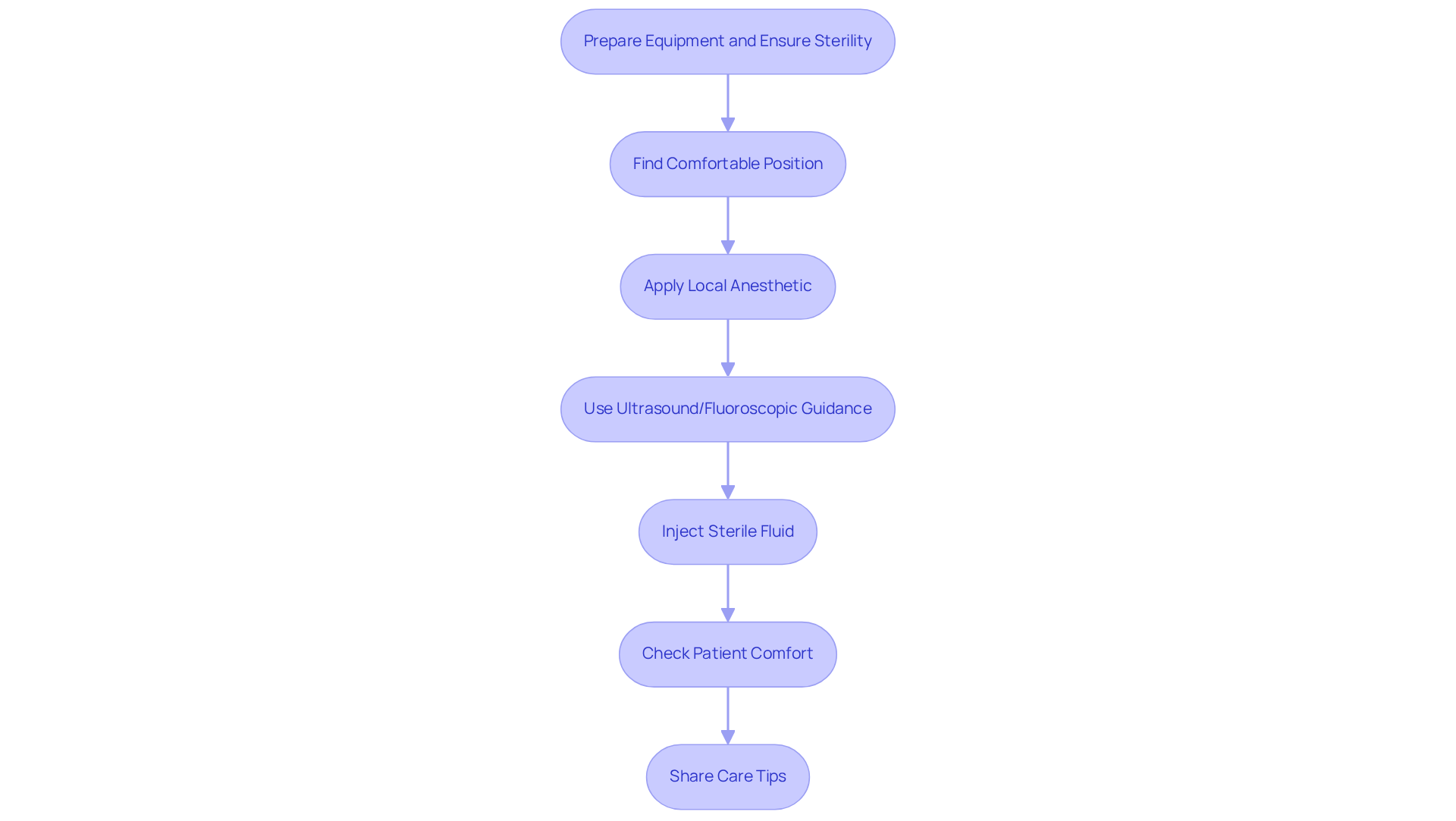
Many individuals facing joint pain often feel anxious about the procedures meant to help them. To effectively perform joint distension, it’s important to have all your equipment ready and sterile, ensuring you feel confident in the procedure ahead.
Making sure you’re comfortable is key, so let’s find a position that feels right for you. For shoulder distension, you might prefer to be seated or lying down, depending on what feels best for you.
To help ease any discomfort, we’ll gently apply a local anesthetic to the area. This way, you can focus on the relief that’s coming.
We’ll use ultrasound or fluoroscopic guidance to ensure we’re in the right spot, giving you peace of mind. This careful approach helps us confirm that we’re in the right place before we proceed.
Next, we’ll carefully inject the sterile fluid into your joint, while monitoring for any signs of joint distension throughout the process. It’s important to us that you’re comfortable, so we’ll adjust the injection speed if needed.
Once the injection is done, we’ll check in with you to see how you’re feeling and address any concerns. Your comfort and safety are our top priorities.
Finally, we’ll share some care tips to help you recover smoothly and feel your best. At RegenCore, our customized regenerative treatments, which use naturally sourced cell-based biologics, further improve healing and recovery for individuals facing inflammation and swelling. Statistics suggest that patients frequently feel instant relief from discomfort and a return to near-normal function after the operation, emphasizing the significance of appropriate technique and patient care. With the right care and technique, patients can not only alleviate their pain but also regain their confidence in movement.
Troubleshoot Common Issues: Managing Complications in Joint Distension
Even when procedures are designed to be safe, the unexpected can happen, leaving patients feeling vulnerable and concerned. Here are some common issues you might face and effective ways to manage them:
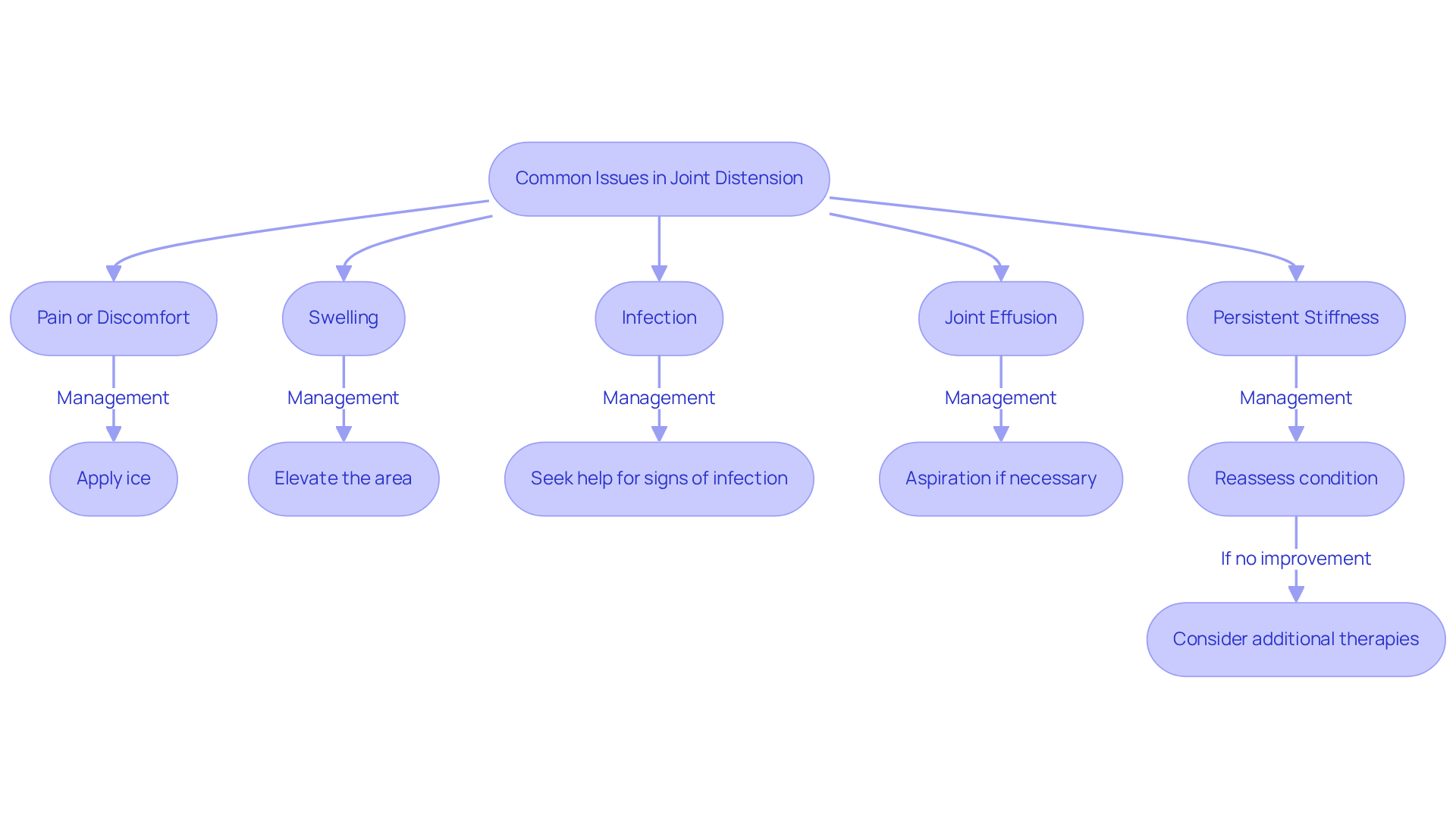
- Pain or Discomfort: If you’re feeling discomfort, applying ice can be a soothing relief. It’s not uncommon to experience increased pain after the procedure. If the pain persists for more than one to two weeks, it’s important to reach out for further evaluation. Remember, you’re not alone in this; many have walked this path and found their way to relief.
- Swelling: Mild swelling is a typical response after tissue distension. Elevating the area and taking it easy for a few days can help minimize discomfort and promote healing. At RegenCore, we understand how important it is to heal, and our personalized regenerative therapies are designed to support you every step of the way, helping to reduce inflammation and enhance your recovery.
- Infection: Although rare, infections can occur at the injection site. Keep an eye out for signs like redness, warmth, or discharge. If you notice any of these symptoms, don’t hesitate to seek help. Early intervention with appropriate antibiotic therapy can prevent complications and give you peace of mind.
- Joint Effusion: Sometimes, excess fluid can build up in the joint after the procedure. If this happens, aspiration might be necessary to relieve pressure and discomfort. RegenCore’s innovative regenerative therapies address the underlying issues that contribute to fluid accumulation, ensuring a comprehensive approach to your recovery.
- Persistent Stiffness: If you’re not seeing improvement in your range of motion, it’s essential to reassess your condition. Additional therapies, like physical therapy or further injections, may be needed to effectively address ongoing stiffness. At RegenCore, we offer a range of regenerative options tailored to your individual needs, enhancing treatment effectiveness and promoting tissue repair.
By proactively addressing these common complications, you can enhance the overall effectiveness of joint distension and facilitate a smoother recovery process. Understanding these potential challenges and knowing that support is available can help you navigate your recovery with confidence and hope.
Conclusion
Imagine waking up every day, unable to move your shoulder without pain – this is the reality for many suffering from frozen shoulder. Mastering joint distension can be a game-changer for healthcare professionals looking to help these patients reclaim their mobility and quality of life. With hydrodilatation techniques, healthcare providers can help patients rediscover the joy of movement and the freedom to engage in life fully. This minimally invasive procedure not only reduces pain significantly but also enhances the range of motion, allowing individuals to participate in their daily activities without discomfort.
Throughout this guide, we’ve explored the key aspects of joint distension, emphasizing the importance of thorough patient assessments and the step-by-step procedure for effective execution. Each phase, from gathering a comprehensive client history to providing post-procedure care, plays a crucial role in ensuring the success of the treatment. Understanding these components empowers professionals to deliver tailored care that meets the unique needs of each patient, ultimately leading to improved outcomes.
Mastering joint distension isn’t just about technique; it’s about showing our patients that we care and are dedicated to their healing journey. As healthcare providers embrace these techniques, they not only transform individual lives but also contribute to the broader landscape of pain management and rehabilitation. By prioritizing ongoing education and patient-centered care, you can make a lasting impact on your patients’ journeys toward pain-free movement and restored vitality. As you embrace these techniques, remember that each patient you help is a step toward a future where pain no longer dictates their lives.
Frequently Asked Questions
What is hydrodilatation?
Hydrodilatation is a minimally invasive technique that involves injecting sterile fluid into the joint space to expand it and relieve stiffness, particularly for those suffering from frozen shoulder or adhesive capsulitis.
How does hydrodilatation help with frozen shoulder?
Hydrodilatation helps alleviate the pain and stiffness associated with frozen shoulder, allowing patients to regain mobility and improve their ability to move without discomfort.
What improvements have been reported following hydrodilatation?
Research shows significant improvements, including a reduction in pain from a mean Visual Analog Scale (VAS) score of 7.97 to 0.4 over two years, and an improvement in the mean Disabilities of the Arm, Shoulder, and Hand (DASH) score from 47.42 to 1.6.
What percentage of individuals may require reintervention after hydrodilatation?
A cohort study indicated that about 24.7% of individuals may need reintervention after undergoing hydrodilatation.
What are the overall benefits of understanding joint distension for healthcare providers?
By understanding the mechanics and benefits of joint distension, healthcare providers can better assess its relevance for their patients, leading to improved outcomes in joint health and mobility.
List of Sources
- Understand Joint Distension: Definition and Importance
- Predictors of reintervention following hydrodistension as a treatment for adhesive capsulitis | Bone & Joint (https://boneandjoint.org.uk/Article/10.1302/2633-1462.69.BJO-2025-0001.R1)
- Long-Term Outcomes of Ultrasound-Guided Hydrodistension for Adhesive Capsulitis: A Prospective Observational Study (https://mdpi.com/2379-139X/9/5/147)
- Additive effect of glenohumeral joint hydrodilatation applied in addition to suprascapular nerve blockage in patients with adhesive capsulitis – BMC Musculoskeletal Disorders (https://link.springer.com/article/10.1186/s12891-024-08082-w)
- Updates on the treatment of adhesive capsulitis with hydraulic distension (https://e-jyms.org/journal/view.php?doi=10.12701/yujm.2020.00535)
- Prepare for Joint Distension: Assessments and Evaluations
- Functional Outcome of Hydrodilation in Adhesive Capsulitis of Shoulder (https://jocr.co.in/wp/2025/05/functional-outcome-of-hydrodilation-in-adhesive-capsulitis-of-shoulder)
- Long-Term Outcomes of Ultrasound-Guided Hydrodistension for Adhesive Capsulitis: A Prospective Observational Study (https://mdpi.com/2379-139X/9/5/147)
- Hydrodilatation (Joint Distention) | Pain Treatment Procedure (https://paincareflorida.com/pain-care-treatments/hydrodilatation-joint-distention)
- Distension arthrogram in the treatment of adhesive capsulitis has a low rate of repeat intervention | Bone & Joint (https://boneandjoint.org.uk/Article/10.1302/0301-620X.102B5.BJJ-2020-0082)
- The effectiveness of ultrasound guided hydrodistension and physiotherapy in the treatment of frozen shoulder/adhesive capsulitis in primary care: a single centre service evaluation – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5598823)
- Execute Joint Distension: Step-by-Step Procedure
- Joint Distension | Main Line Health (https://mainlinehealth.org/conditions-and-treatments/treatments/joint-distension)
- Frozen Shoulder Treatments: Complete Evidence Guide | San Jose (https://jeffreypengmd.com/post/frozen-shoulder-treatments-that-actually-work-a-complete-evidence-based-guide)
- Arthrographic Distension / Hydrodilatation (https://shoulderdoc.co.uk/pages/arthrographic-distension-hydrodilatation)
- Hydrodilatation (Joint Distention) | Pain Treatment Procedure (https://paincareflorida.com/pain-care-treatments/hydrodilatation-joint-distention)
- Shoulder Hydrodilatation | RYC Orthopaedics, Sports Medicine Expert, NY (https://rycorthopaedics.com/shoulder-hydrodilatation-orthopaedic-treatments-new-york)
- Troubleshoot Common Issues: Managing Complications in Joint Distension
- Millions with joint pain and osteoarthritis are missing the most powerful treatment (https://sciencedaily.com/releases/2026/03/260303145725.htm)
- Scientists discover new clues about joint disease and possible treatments (https://ohio.edu/news/2025/09/scientists-discover-new-clues-about-joint-disease-possible-treatments)
- 7 Reasons You Might Be Experiencing Joint Pain, According to an Expert (https://today.com/health/aging/joint-pain-telling-health-rcna215024)
- Complications to 6 months following total hip or knee arthroplasty: observations from an Australian clinical outcomes registry – BMC Musculoskeletal Disorders (https://link.springer.com/article/10.1186/s12891-020-03612-8)

