Introduction
Navigating the landscape of arthritis pain management can feel overwhelming, especially when faced with the choice between nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids. Each of these medication classes offers unique benefits in relieving discomfort, yet they also carry their own risks.
For many, the struggle is real: how do you find the right balance between effective pain relief and the potential dangers that come with each option?
This article takes a compassionate look at the comparative analysis of NSAIDs and opioids, shedding light on their effectiveness, limitations, and the evolving strategies that can help manage arthritis pain.
Understanding Arthritis Pain Management: NSAIDs vs. Opioids
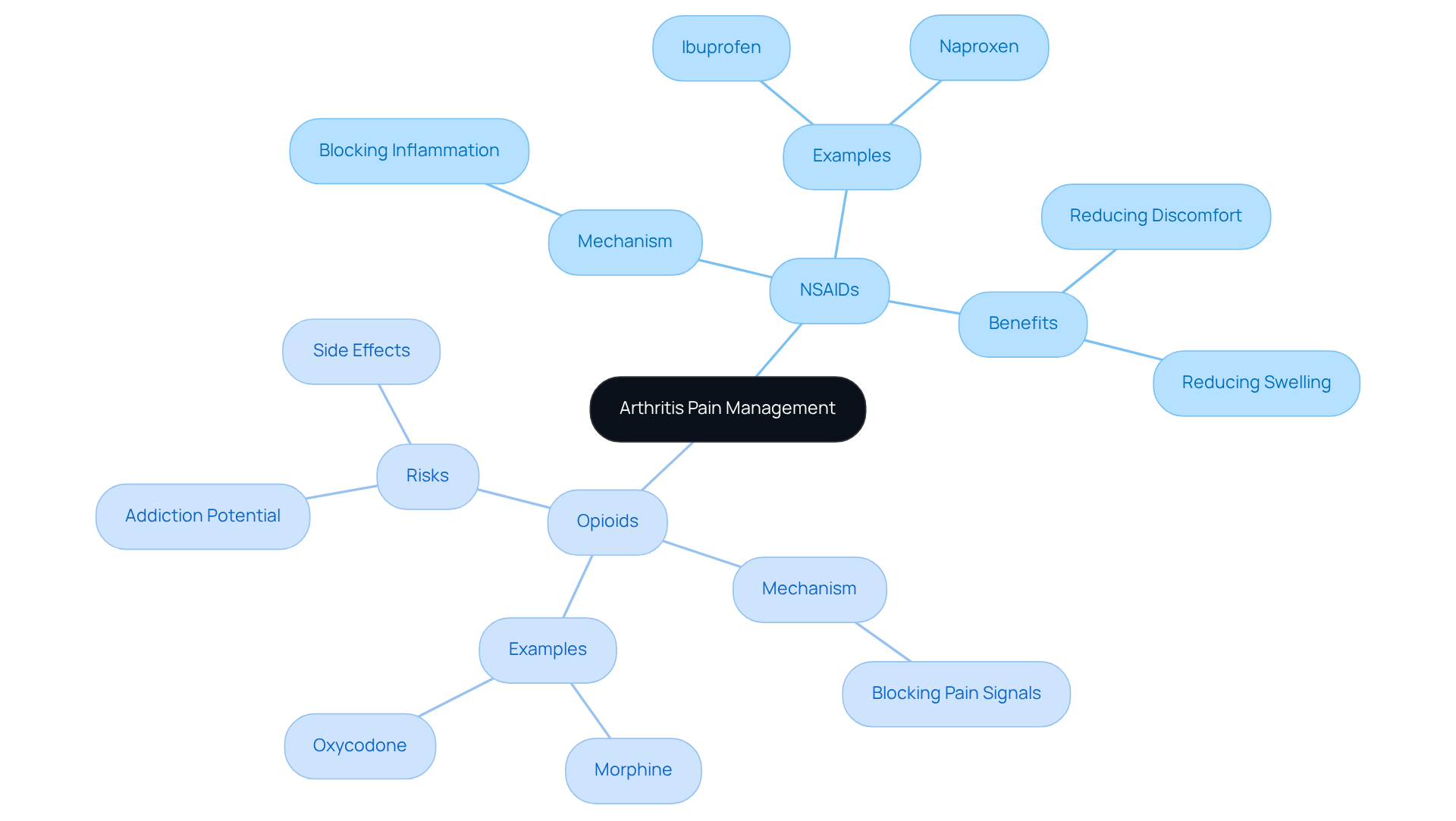
Managing arthritis pain pills for discomfort can feel overwhelming, especially when it comes to choosing the right treatment. Many individuals find themselves navigating the complexities of nonsteroidal anti-inflammatory medications (NSAIDs) and opioids, each serving a unique purpose in their journey toward relief. NSAIDs, like ibuprofen and naproxen, work by blocking the enzymes that lead to inflammation, helping to ease both discomfort and swelling. For those dealing with mild to moderate pain linked to inflammatory conditions, arthritis pain pills often become a go-to option, offering a sense of hope and relief.
On the other hand, opioids such as morphine and oxycodone target the central nervous system to block pain signals, offering a lifeline for those experiencing intense suffering. However, the potential for addiction and significant side effects can make their use a daunting choice, prompting individuals and healthcare providers to weigh the risks carefully. This delicate balance is crucial, as the goal is to find a solution that not only alleviates pain but also supports overall well-being.
Recent data shows that by 2025, many individuals still turn to arthritis pain pills, including NSAIDs, as a first-line treatment for arthritis management. This trend highlights the ongoing conversation about the opioid crisis, which has raised awareness about the importance of responsible pain management strategies. Pain management specialists emphasize the need for personalized treatment plans that may include arthritis pain pills, considering each person’s unique needs. While NSAIDs may work wonders for many, there are those who find that opioids are the only option that truly addresses their severe discomfort, as illustrated by various case studies of individuals who have explored different avenues for relief.
Understanding the therapeutic mechanisms behind NSAIDs and opioids is essential for making informed decisions about treatment. NSAIDs primarily target inflammation, while opioids focus on modulating pain signals. This distinction is vital for individuals to grasp as they discuss their options with healthcare providers. As the landscape of arthritis discomfort relief continues to evolve, staying informed about the latest developments in medication efficacy and safety is key to optimizing outcomes and enhancing the quality of life.
Exploring NSAIDs: Benefits and Limitations in Arthritis Treatment
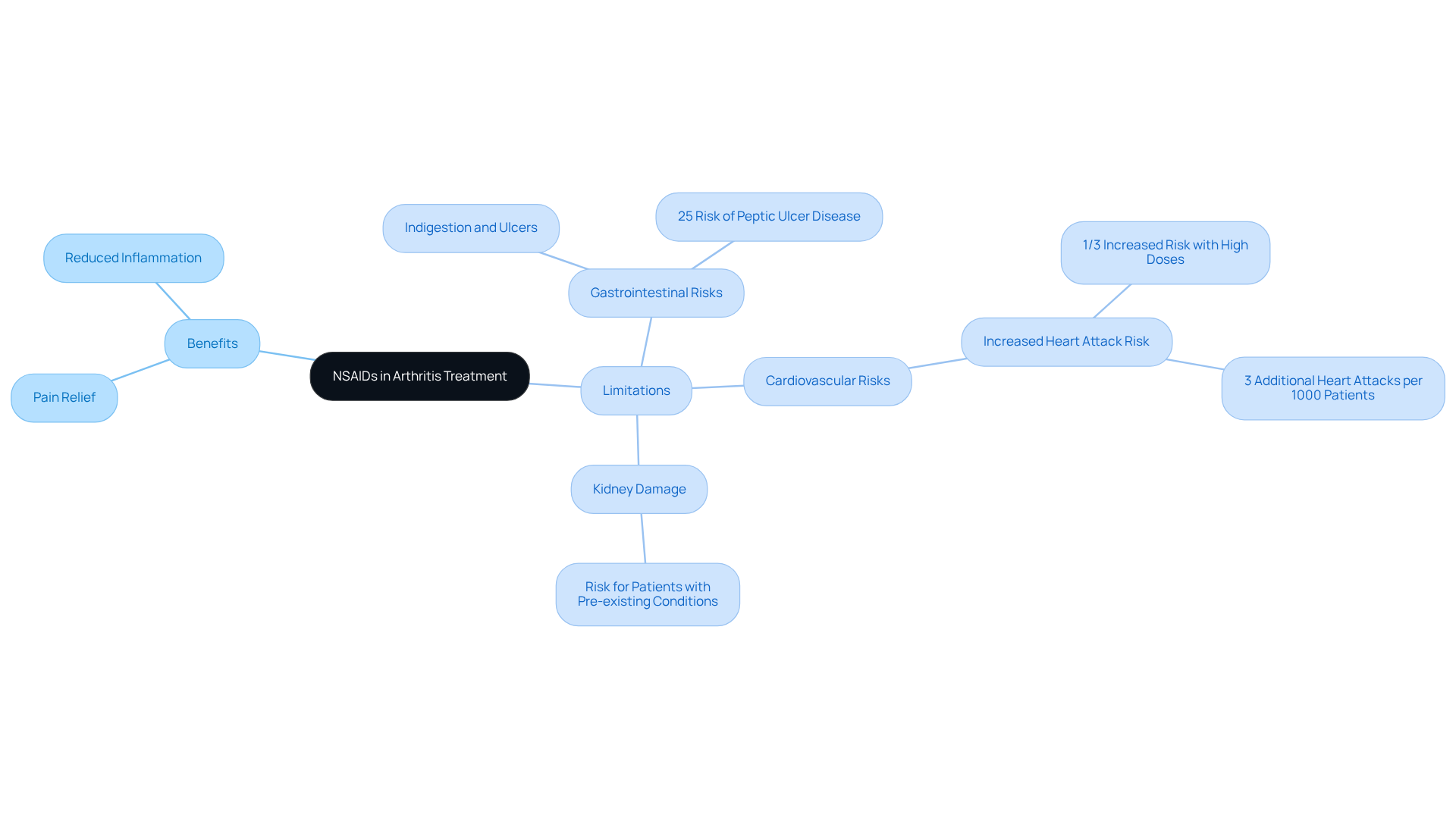
Living with arthritis pain pills can be a daily struggle, filled with discomfort and frustration. Arthritis pain pills, such as nonsteroidal anti-inflammatory drugs (NSAIDs), often serve as a go-to solution for many, providing relief from pain and reducing inflammation. Their easy availability over-the-counter makes them a popular choice for those seeking to manage mild to moderate pain. Yet, it’s important to recognize that these medications come with their own set of challenges.
Many individuals may experience gastrointestinal side effects, such as indigestion and ulcers. In fact, studies suggest that around 25% of those who use NSAIDs chronically might develop peptic ulcer disease. This can add another layer of worry for patients already dealing with the pain of arthritis. Moreover, recent research has shed light on the cardiovascular risks tied to prolonged NSAID use. High doses of medications like diclofenac and ibuprofen have been shown to increase the risk of heart attacks by about one-third, which is a significant concern for anyone managing their health.
Kidney damage is yet another potential risk, especially for those with pre-existing conditions. While arthritis pain pills can help manage symptoms, they don’t tackle the root causes of arthritis. This is where the conversation becomes crucial. Patients are encouraged to engage openly with their healthcare professionals, discussing not just the benefits of NSAIDs but also the possible risks. Together, they can explore alternative or adjunct therapies that may offer a more comprehensive approach to treatment, tailored to each individual’s unique health profile.
Ultimately, it’s about finding a balance that works for you. By participating in these discussions, patients can customize their management strategies, ensuring they address both their symptoms and their overall well-being.
Evaluating Opioids: Effectiveness and Risks in Pain Relief
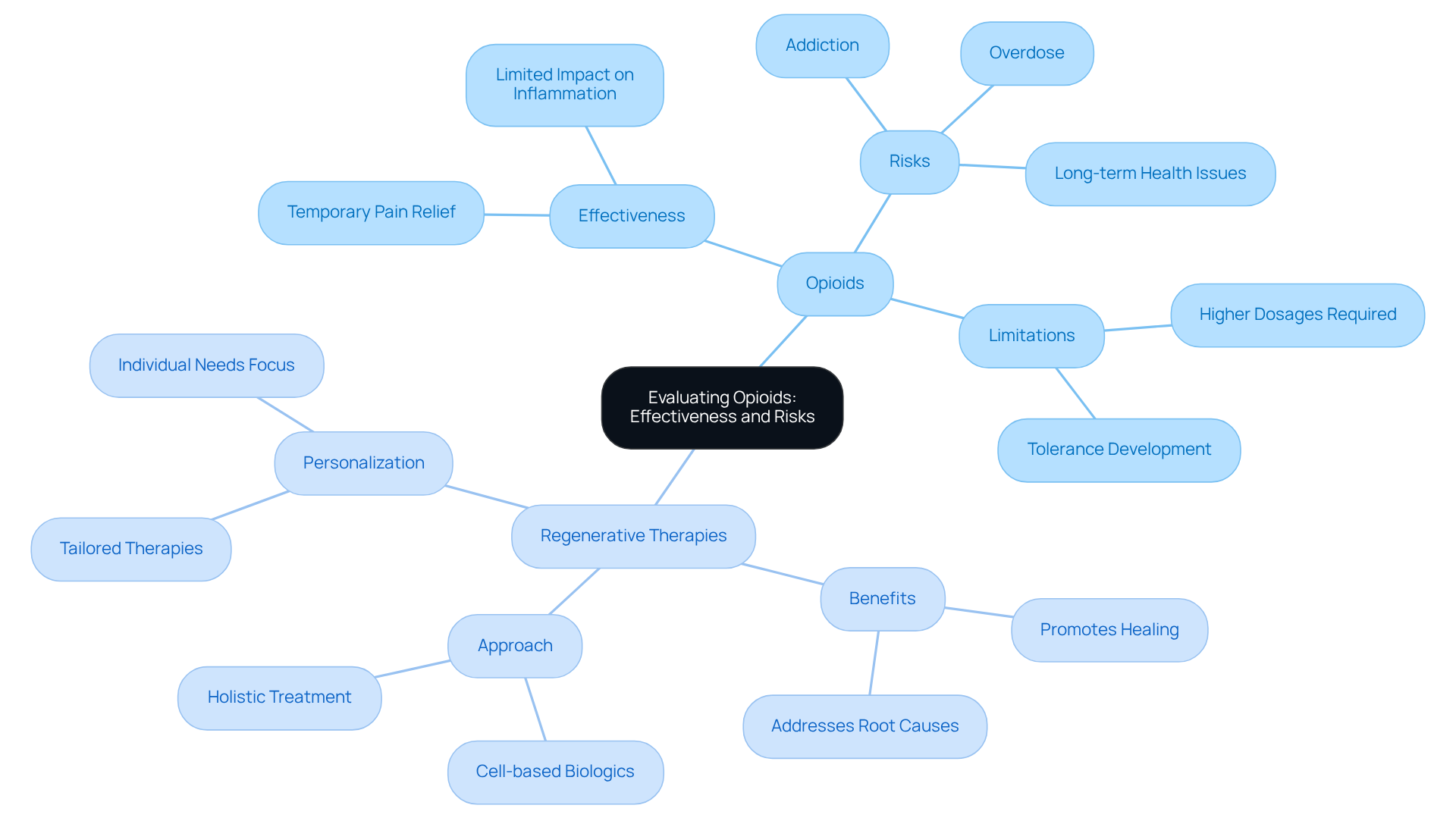
For many patients grappling with severe arthritis pain, arthritis pain pills can seem like a beacon of hope, especially when other treatments have fallen short. Yet, this relief often comes with significant risks – addiction, overdose, and long-term health issues loom large. Research shows that while these painkillers may provide temporary respite, they fail to tackle inflammation, a crucial aspect of arthritis. Moreover, the risk of developing tolerance can lead to higher dosages, increasing the likelihood of adverse effects. This reality underscores the importance of viewing opioids, such as arthritis pain pills, as a last resort in pain management, urging a reduction in their use whenever possible.
At RegenCore, we understand the struggles faced by those with arthritis, and we’re here to offer a compassionate alternative. Our personalized regenerative therapies harness the power of naturally derived cell-based biologics to promote healing and repair tissue damage in arthritic or injured joints. These innovative therapies provide a safe and effective substitute for narcotics, focusing on enhancing recovery and addressing the root causes of joint pain, which is often treated with arthritis pain pills. By employing a variety of regenerative modalities tailored to each individual’s needs, we strive to create a holistic approach to joint health that prioritizes lasting healing over mere temporary relief.
Comparative Analysis: Pros and Cons of NSAIDs and Opioids
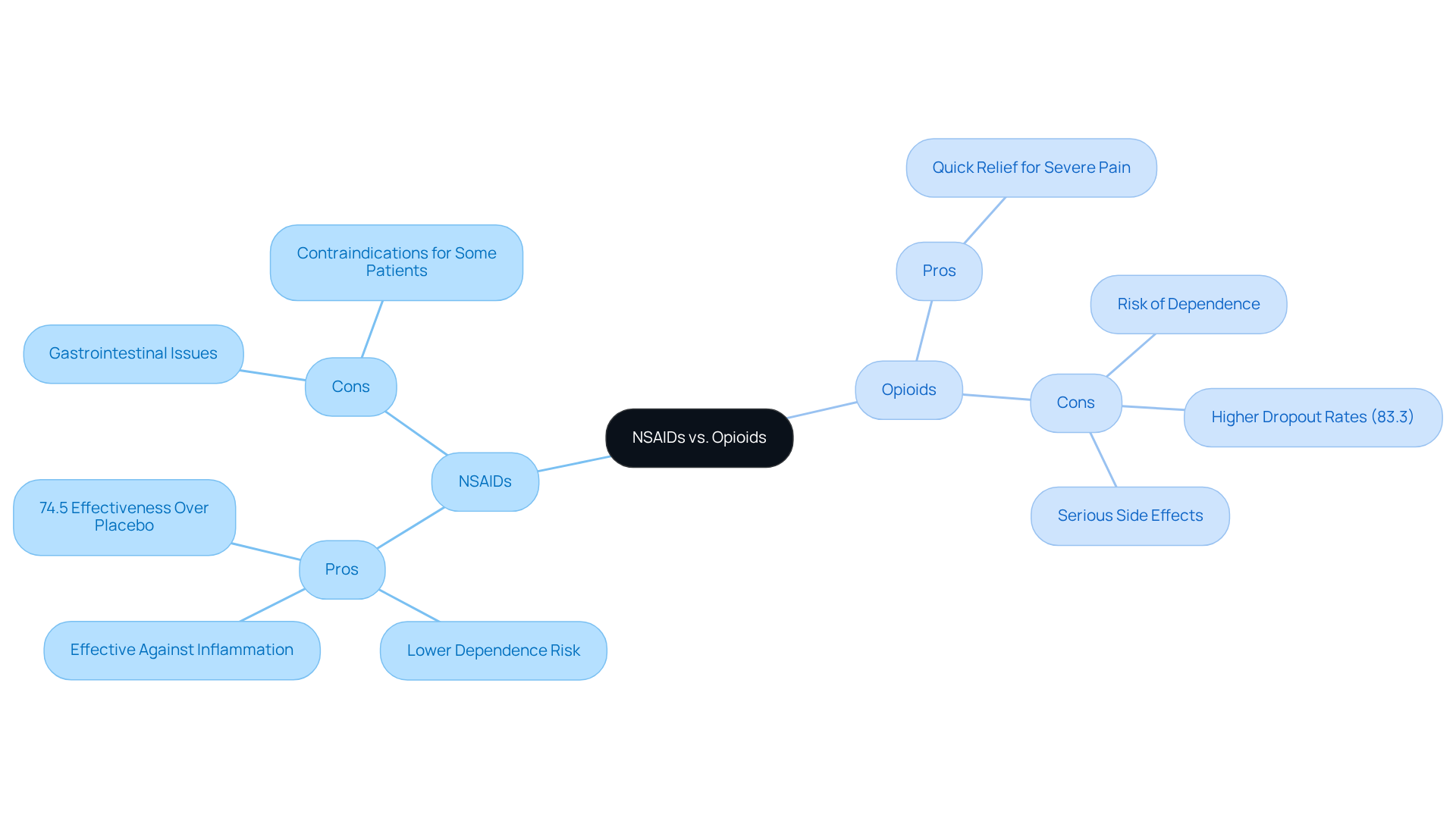
When it comes to managing arthritis discomfort, the choice between non-steroidal anti-inflammatory drugs (NSAIDs) and opioids can feel overwhelming. Many people suffering from arthritis know all too well the relentless pain that can accompany this condition. NSAIDs, celebrated for their anti-inflammatory properties, often emerge as the first line of defense. They effectively tackle pain linked to inflammation, and recent studies reveal that a remarkable 74.5% of oral NSAIDs outperform placebos, reinforcing their status as a go-to option. Patients often prefer them due to a lower risk of dependence compared to opioids, though it’s important to acknowledge that gastrointestinal issues and certain contraindications can limit their use for some individuals.
On the other hand, while opioids can provide quick relief for severe pain, they come with significant risks. Dependence and serious side effects can make them a less favorable choice for long-term management. Their use is typically reserved for short-term situations, especially during acute pain episodes. A striking clinical trial highlighted that individuals opting for non-opioid treatments reported better pain intensity outcomes over a year compared to those using opioids. Moreover, the dropout rates due to adverse events were alarmingly higher among narcotic users, with 83.3% experiencing increased dropout rates compared to just 18.5% of those using oral NSAIDs.
Experts emphasize that the decision to use NSAIDs or opioids should be tailored to each person’s unique situation, taking into account the severity of their pain, medical history, and potential side effects. As Dr. James Slauterbeck wisely points out, prioritizing non-opioid pain management strategies can significantly reduce the risks associated with opioid use while still providing effective relief. This compassionate, multimodal approach-often involving scheduled doses of acetaminophen alongside NSAIDs-is increasingly recommended in clinical practice, aiming to enhance both outcomes and safety for those navigating the challenges of arthritis.
Personalizing Pain Management: Integrating Alternative Therapies
For many individuals living with arthritis, the pain can feel overwhelming, often leading them to seek arthritis pain pills for relief. Traditional treatments such as arthritis pain pills, including NSAIDs and opioids, may offer some help, but they come with their own set of challenges and side effects. This is where alternative therapies step in, providing a beacon of hope for those seeking a more holistic approach to pain management.
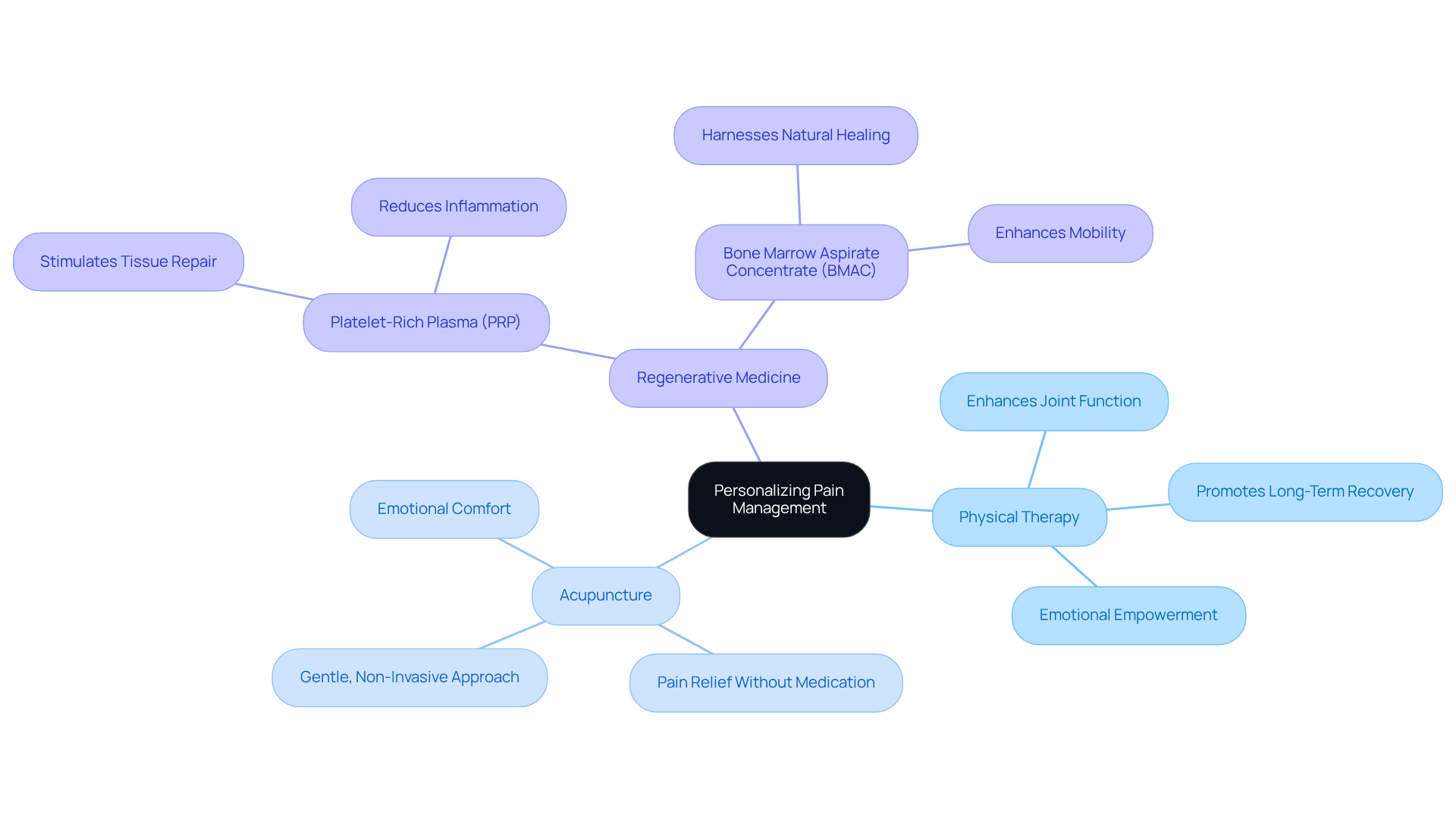
Imagine being able to move freely again, to engage in activities you love without the constant reminder of discomfort. Physical therapy offers just that. It not only enhances joint function and mobility but also empowers individuals to partake in tailored exercises that promote long-term recovery. This journey towards healing is not just physical; it’s emotional, too. The sense of accomplishment and renewed strength can be life-changing.
Acupuncture, another alternative therapy, has gained recognition for its gentle, non-invasive approach to alleviating pain. Many patients have shared their stories of finding relief through this ancient practice, often noting how it helps them manage discomfort without the risks associated with arthritis pain pills. It’s a comforting thought to know that there are options available that prioritize your well-being.
At RegenCore, we understand the importance of these innovative therapies. Recent advancements in regenerative medicine, particularly with Platelet-Rich Plasma (PRP) and Bone Marrow Aspirate Concentrate (BMAC), have shown remarkable promise. These techniques harness the body’s natural healing abilities, stimulating tissue repair and reducing inflammation. By integrating these therapies into a personalized pain management plan, patients can not only improve their outcomes but also enhance their overall quality of life. This shift towards a more holistic approach in arthritis treatment reflects a growing understanding of the need for compassionate care that addresses both the physical and emotional aspects of pain.
Conclusion
Navigating the landscape of arthritis pain management can feel overwhelming, especially when faced with the choice between NSAIDs and opioids. Many individuals grapple with the challenge of finding effective relief, and understanding the differences between these medications is crucial for making informed decisions about their pain management strategies.
NSAIDs are often a go-to for those dealing with mild to moderate pain, primarily because they target inflammation and come with a lower risk of dependence. However, for those experiencing severe pain, opioids may seem like a tempting option due to their ability to provide quick relief. Yet, this relief comes with significant risks, including the potential for addiction and other adverse side effects. It’s essential to recognize that each person’s journey is unique, and personalized treatment plans that consider individual health profiles and pain levels are vital. Open dialogue between patients and healthcare providers can foster a supportive environment where concerns are addressed, and the best path forward is determined.
Ultimately, the journey toward effective arthritis pain management is multifaceted and deeply personal. Exploring alternative therapies and innovative treatments, such as regenerative medicine, can not only enhance outcomes but also significantly improve quality of life. Embracing a holistic approach to pain management addresses not just the physical symptoms but also nurtures emotional well-being. This empowers individuals to reclaim their lives from the grip of arthritis pain, fostering hope and resilience in their ongoing journey.
Frequently Asked Questions
What are NSAIDs and how do they work for arthritis pain management?
Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, work by blocking enzymes that lead to inflammation, helping to ease both discomfort and swelling associated with arthritis.
When are opioids recommended for arthritis pain?
Opioids, like morphine and oxycodone, are recommended for individuals experiencing intense pain that NSAIDs cannot adequately manage, as they target the central nervous system to block pain signals.
What are the risks associated with opioid use in pain management?
The use of opioids carries the potential for addiction and significant side effects, making it a daunting choice for many individuals and prompting careful consideration by healthcare providers.
Why is it important to have personalized treatment plans for arthritis pain management?
Personalized treatment plans are essential because they consider each individual’s unique needs and circumstances, allowing for a more effective approach to managing pain and supporting overall well-being.
What are some common side effects of NSAIDs?
Common side effects of NSAIDs include gastrointestinal issues such as indigestion and ulcers, with studies suggesting that around 25% of chronic NSAID users may develop peptic ulcer disease.
What cardiovascular risks are associated with prolonged NSAID use?
Prolonged use of high doses of NSAIDs like diclofenac and ibuprofen has been shown to increase the risk of heart attacks by about one-third.
How can patients manage the risks of NSAIDs while treating arthritis?
Patients are encouraged to engage in open discussions with their healthcare professionals about the benefits and risks of NSAIDs, exploring alternative or adjunct therapies for a more comprehensive treatment approach.
Do NSAIDs address the root causes of arthritis?
No, while NSAIDs can help manage symptoms of arthritis, they do not tackle the underlying causes of the condition.
