Introduction
Understanding the complexities of the iliotibial band (ITB) is crucial for athletes who want to boost their performance and avoid injuries. This important structure not only stabilizes the knee during movement but also plays a key role in how forces are transmitted and in maintaining posture. Yet, many find themselves struggling with IT band syndrome, facing frustrating symptoms that can disrupt their active lives.
How can athletes navigate the challenges of ITB anatomy and management to stay at the peak of their game?
Understand the Iliotibial Band: Anatomy and Function
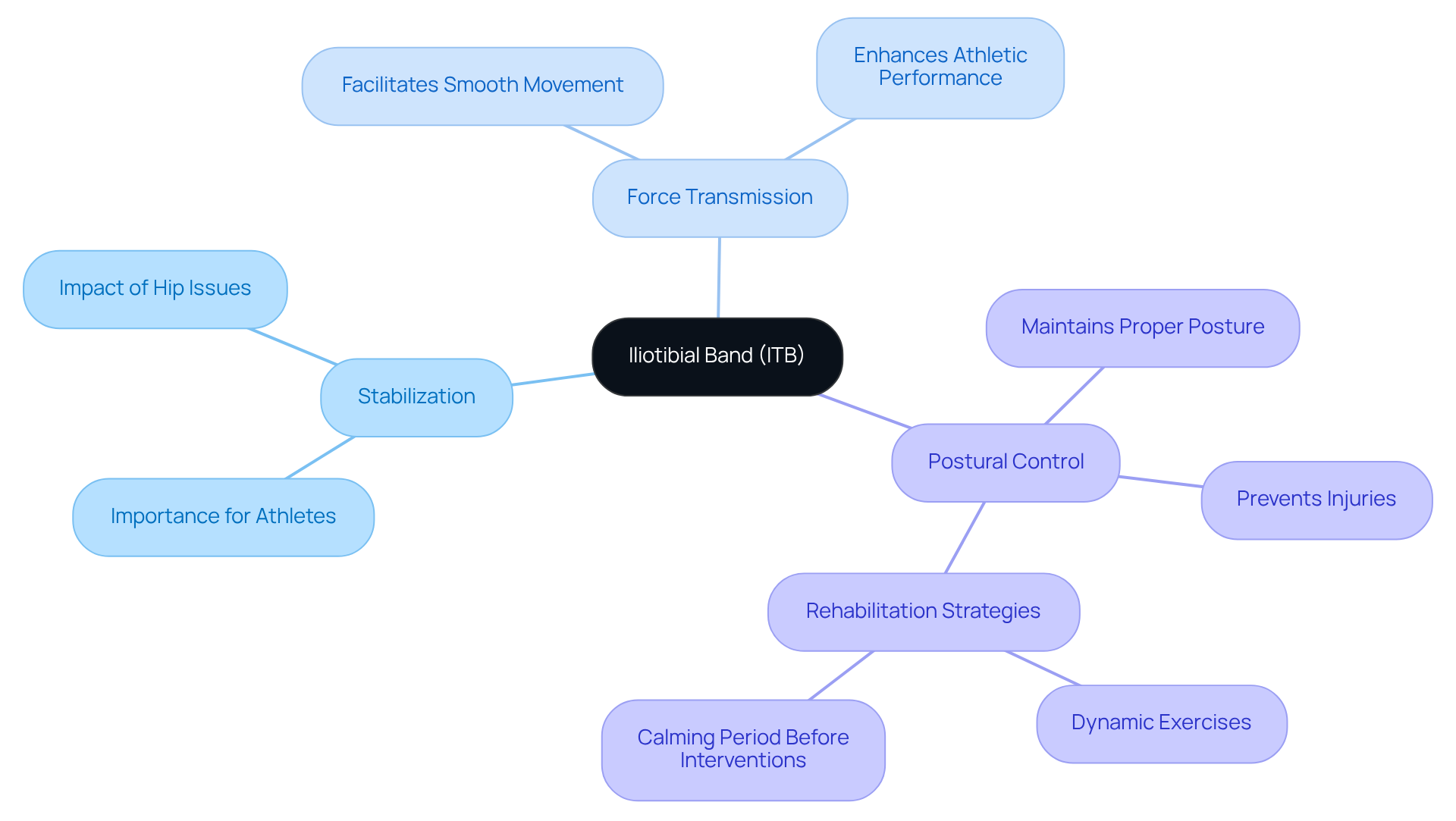
The iliotibial band (ITB) is more than just a band of connective tissue; it’s a crucial support system that runs along the outer thigh, emphasizing the importance of stability, starting from the iliac crest and connecting to the lateral condyle of the tibia. For many, this structure is vital for stability during activities like running and cycling. Formed from the fascia lata, which envelops the thigh muscles including the gluteus maximus and tensor fasciae latae, the ITB has several important roles:
- Stabilization: The ITB is key in keeping the knee stable, preventing excessive lateral movement. This stability is especially important for athletes engaged in dynamic sports, where every movement counts.
- Force Transmission: It efficiently transmits forces from the hip to the leg, which not only facilitates smooth movement but also enhances athletic performance.
- Postural Control: The ITB helps maintain proper posture during physical activities, which is essential for optimal biomechanics and preventing injuries.
However, many individuals experience discomfort related to the ITB, often feeling frustrated and limited in their activities. Recent studies have underscored the importance of the ITB in athletic performance, revealing that issues at the hip can significantly affect its function. This can lead to pain and hinder athletic abilities, leaving many feeling disheartened. Research indicates that targeted interventions can alleviate ITB-related discomfort and improve overall joint stability. Understanding the ITB’s anatomy is crucial for athletes who aim to prevent injuries and enhance their performance.
At RegenCore, we recognize the challenges faced by those dealing with ITB issues. We offer innovative therapies, such as physical therapy and manual therapy. These therapies harness the body’s natural healing processes to support recovery from injuries. Our personalized approach targets the ITB’s functions, promoting tissue repair and reducing inflammation, ultimately providing athletes with tailored solutions to manage pain and enhance performance.
Incorporating targeted rehabilitation strategies, like dynamic exercises and a calming period before active interventions, can further assist in managing ITB-related concerns. We’re here to support you on your journey to recovery, helping you regain your strength and confidence.
Identify IT Band Syndrome: Symptoms and Causes
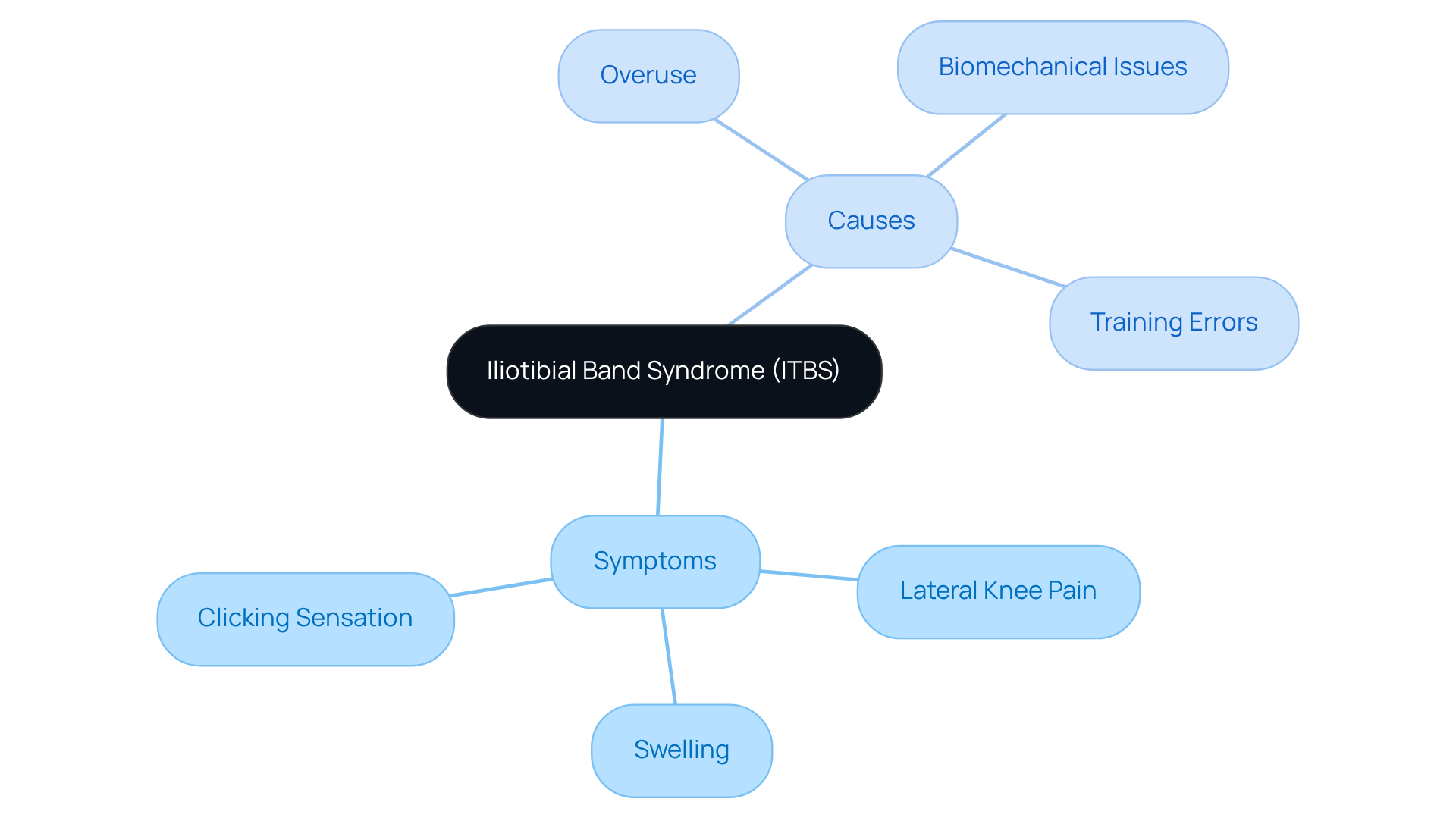
(ITBS) can be a frustrating and painful experience, often manifesting as sharp or burning pain on the outer side of the knee. For many, this discomfort can feel overwhelming, especially when it disrupts daily activities. Key symptoms include:
- Pain: This pain often worsens during activities like running, cycling, or climbing stairs, making it hard to enjoy the things you love.
- Swelling: Inflammation around the joint can add to the discomfort, leaving you feeling restricted.
- Clicking Sensation: Some people notice a clicking or popping sound during movement, a sign that irritation is present.
The causes of ITBS can be just as challenging:
- Overuse: Repetitive activities, especially for runners and cyclists, can lead to irritation of the IT band, leaving you in pain.
- Biomechanical Issues: Factors like poor alignment, leg length discrepancies, or weak hip muscles can increase strain on the IT structure, complicating your recovery.
- Training Errors: Sudden increases in mileage or intensity without proper conditioning can trigger these symptoms, making it crucial to listen to your body.
At RegenCore, we truly understand how conditions like ITBS can impact your life, especially for active professionals. Our personalized treatments harness the power of naturally derived cell-based biologics to promote healing and recovery, offering a safe and effective path to recovery. Recent studies show that ITBS is particularly common among distance runners, with a reported incidence of 1.63% among race entrants. Additionally, a history of allergies and asthma have been identified as independent risk factors for developing ITBS. By understanding these symptoms and causes, athletes can take proactive steps to prevent injuries and enhance performance. At RegenCore, we’re here to support you on your recovery journey, helping you get back to doing what you love.
Diagnose IT Band Syndrome: Assessment Techniques
Diagnosing IT band syndrome can feel overwhelming, and it’s crucial to approach it with care and understanding. Many patients struggle with pain and uncertainty, making it essential to combine clinical assessments with a thorough patient history to uncover the root of their discomfort.
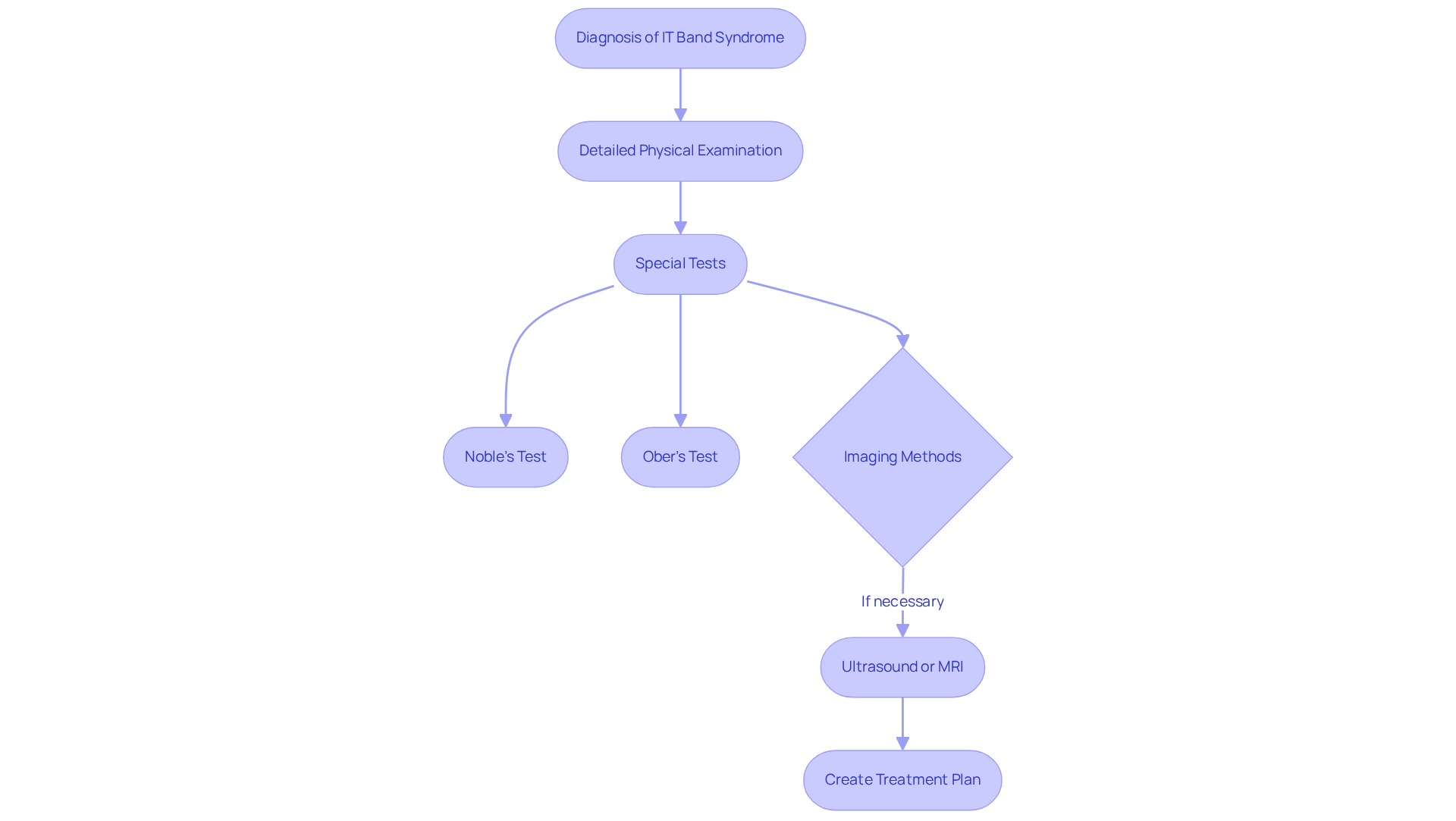
A detailed physical examination is a vital first step. By focusing on the knee and hip, healthcare providers can assess tenderness along the IT band and evaluate the range of motion. This examination not only helps identify signs of inflammation or mechanical issues but also reassures patients that their concerns are being taken seriously.
Special tests play a significant role in confirming the diagnosis. Noble’s Test, for instance, involves applying pressure to the IT band while flexing and extending the knee to provoke pain. While this can help confirm the presence of IT band syndrome, recent studies suggest that practitioners should interpret the results with caution, ensuring that patients feel supported throughout the process. Similarly, assessing how well the leg can drop towards the table when the patient lies on their side is important. Though traditionally used, the accuracy of this test has been scrutinized, highlighting the importance of careful clinical judgment and empathy in patient care.
In some cases, imaging studies are necessary to rule out other conditions or verify inflammation of the IT band. These tools can provide valuable insights into the underlying issues contributing to the patient’s symptoms, offering hope and clarity in what can often feel like a confusing journey.
Accurate diagnosis is vital for creating an effective treatment plan tailored to each individual’s needs. Physical therapists emphasize that a comprehensive approach, incorporating both physical examination and patient history, is essential for determining the root causes of IT band issues and guiding suitable interventions. It’s heartening to know that with appropriate non-surgical treatment, about 50 to 90% of individuals with ITBS improve within four to eight weeks. Practitioners should also encourage patients to gradually shift their training intensity, helping them to prevent future occurrences of ITBS and regain control over their physical activities.
Treat IT Band Syndrome: Effective Management Strategies
Managing IT band syndrome can feel overwhelming, but you’re not alone in this journey. Many people struggle with the pain and limitations it brings, and it’s crucial to address these challenges with a compassionate approach.
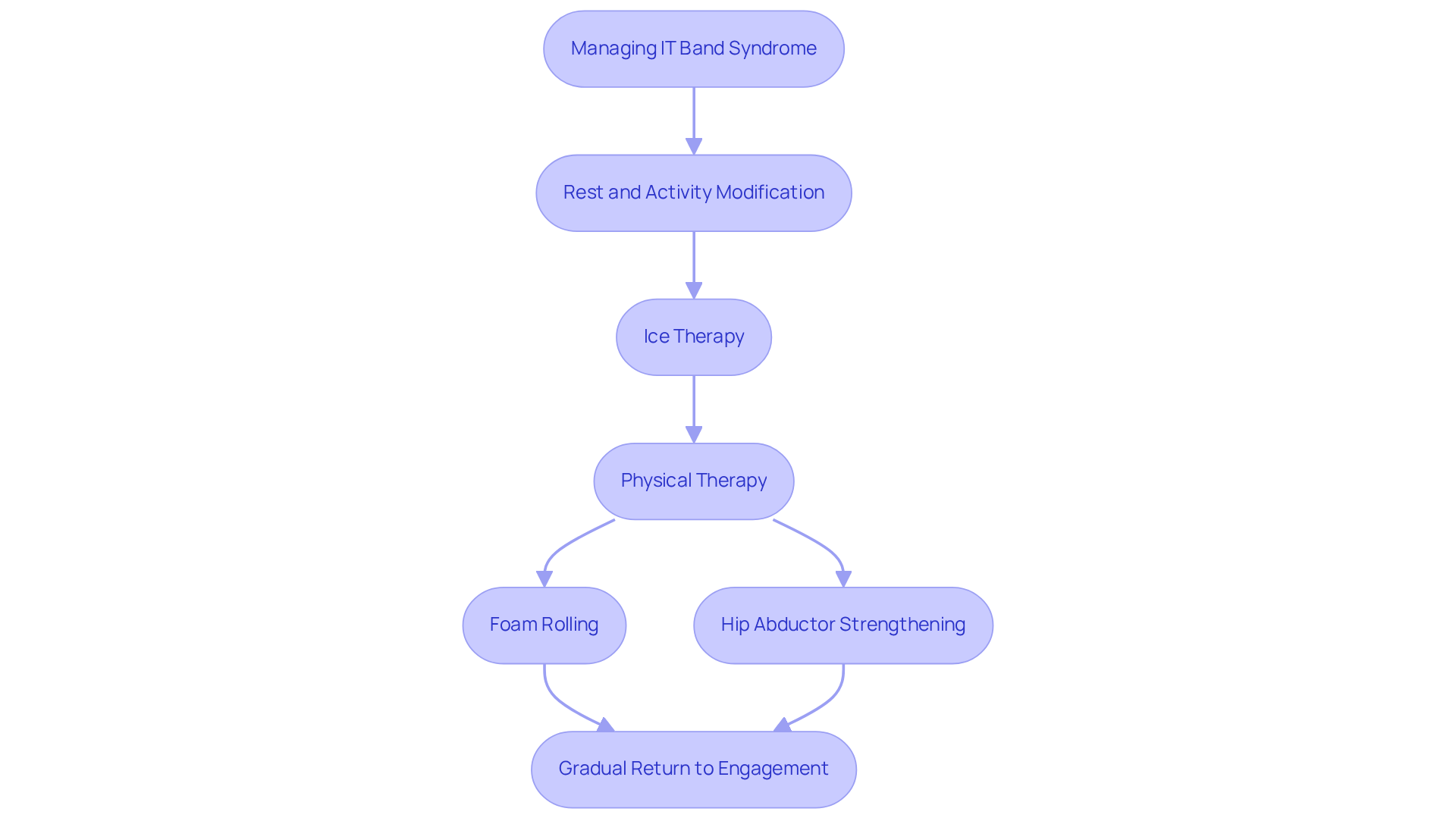
Rest and Activity Modification: One of the first steps is to listen to your body. Reducing or modifying activities that worsen your symptoms is essential for recovery. It’s not about giving up; it’s about finding a way to heal.
Ice Therapy: Applying ice to the affected area can be a simple yet effective way to ease inflammation and pain. This small act of care can promote healing and provide much-needed relief.
Physical Therapy: Engaging in a structured physical therapy program can make a world of difference. Focusing on stretching and strengthening exercises is vital for improving flexibility and muscle balance. Key exercises include:
- Foam Rolling: This technique helps release tension in the IT band and surrounding muscles, enhancing your mobility and comfort.
- Hip Abductor Strengthening: Activities like side-lying leg lifts target the gluteus medius, which can reduce strain on the IT band and improve your overall stability.
Gradual Return: Once you start feeling better, it’s important to ease back into your activities. A gradual return, complete with proper warm-up and cool-down routines, can help prevent re-injury and keep you on the path to recovery.
At RegenCore, we understand the struggles you face. That’s why we offer personalized treatment plans that utilize cell-based biologics to enhance healing and support tissue repair. Backed by research, these innovative therapies can be particularly beneficial for those dealing with issues related to IT band syndrome. By combining these strategies with RegenCore’s therapies, many individuals notice significant improvements within just a few weeks.
In fact, research indicates that with adequate rest and physical therapy, recovery from IT band syndrome can lead to a return to normal activities in about six weeks. Real-world examples show that individuals who engage in focused physical therapy, complemented by RegenCore’s regenerative treatments, often experience a remarkable decrease in symptoms and an improved ability to return to their favorite activities. As Dr. Robert H. Shmerling wisely notes, “Early guidance helps you recover faster and reduces the risk of the problem becoming chronic.” You deserve to feel better, and with the right support, you can achieve that.
Prevent IT Band Syndrome: Practical Tips for Active Professionals
can feel overwhelming, especially for those who love to stay active. The fear of injury can loom large, but with the right approach, you can take control of your training and performance.
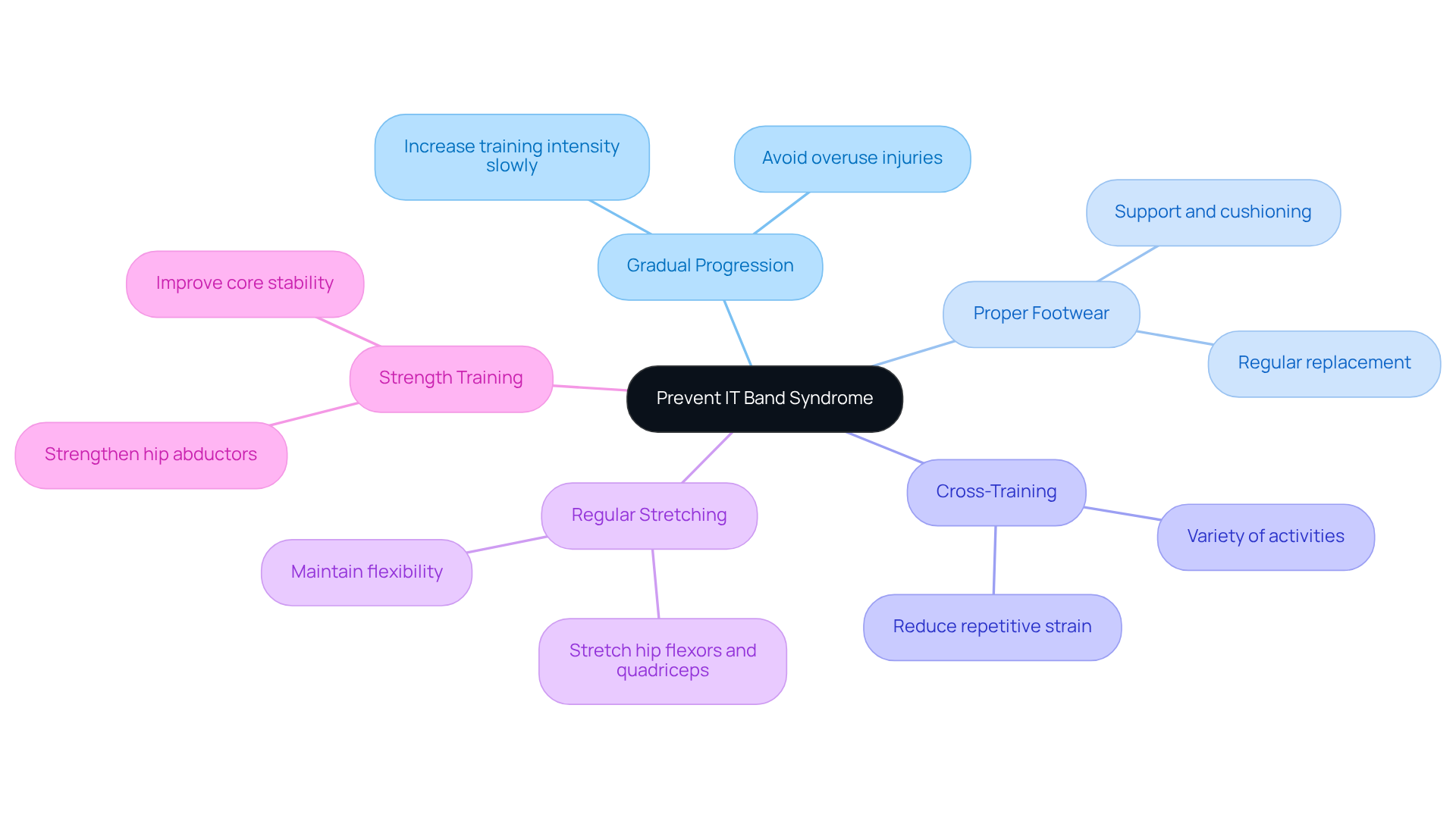
- Consistency is key. It’s tempting to push yourself, but increasing your training intensity and mileage too quickly can lead to overuse injuries. Think of it as a journey; every step counts, and taking your time can make all the difference.
- Footwear plays a crucial role in your comfort and safety. Make sure your shoes offer the support and cushioning you need. Regularly replacing them can prevent wear-related issues that might sneak up on you.
- Cross-Training is another effective strategy. By incorporating a variety of activities, you can reduce repetitive strain on your IT band. This not only keeps your routine fresh but also helps your body adapt and strengthen in different ways.
- Don’t underestimate the power of stretching. Establishing a routine that includes stretching your hip flexors, quadriceps, and the IT band anatomy can help maintain your flexibility. It’s a simple yet powerful way to keep your body in top shape.
- Lastly, focus on strength training. Strengthening your hip abductors and core muscles can significantly improve your stability, reducing the risk of injury. It’s about building a strong foundation that supports your active lifestyle.
By embracing these preventive measures, you can significantly lower your risk of developing IT band syndrome. Remember, it’s not just about avoiding injury; it’s about enhancing your overall performance and enjoying every moment of your active journey.
Conclusion
Mastering the anatomy and function of the iliotibial band (ITB) is crucial for athletes and active individuals. The challenges posed by IT band syndrome can be daunting, often leading to frustration and pain. Understanding the ITB’s role in stability, force transmission, and postural control is not just about performance; it’s about reclaiming the joy of movement and preventing injuries that can sideline you.
Throughout this journey, we’ve explored the symptoms and causes of IT band syndrome, diagnosis techniques, and effective management strategies. Recognizing signs like lateral knee pain and swelling can feel overwhelming, but it’s empowering to know that understanding these underlying biomechanical factors allows you to take proactive steps toward recovery. Treatment options, including:
- Rest
- Physical therapy
- Innovative regenerative therapies
pave the way for healing and can help restore your athletic performance.
Ultimately, embracing preventive measures such as:
- Gradual training progression
- Proper footwear
- Regular strength training
can significantly lower the risk of developing IT band syndrome. By prioritizing these strategies, you can enhance your performance and enjoy your activities without the constant worry of injury. Adopting a holistic approach to ITB health not only fosters a more resilient body but also allows you to continue participating in the sports and activities that bring you joy and fulfillment.
Frequently Asked Questions
What is the iliotibial band (ITB) and where is it located?
The iliotibial band (ITB) is a crucial band of connective tissue that runs along the outer thigh, starting from the iliac crest and connecting to the lateral condyle of the tibia.
What are the main functions of the iliotibial band?
The ITB serves several important roles, including stabilization of the knee to prevent excessive lateral movement, efficient force transmission from the hip to the leg for smooth movement, and postural control during dynamic activities.
What issues can arise related to the iliotibial band?
Many individuals experience discomfort related to the ITB, which can lead to pain and hinder athletic abilities. Issues at the hip can significantly affect ITB function, resulting in frustration and limitations in activities.
How can strengthening hip muscles help with ITB-related discomfort?
Research indicates that strengthening hip muscles can alleviate ITB-related discomfort and improve overall joint stability, helping to prevent injuries and enhance athletic performance.
What are the symptoms of iliotibial band syndrome (ITBS)?
Key symptoms of ITBS include lateral knee pain that worsens during activities like running or cycling, swelling around the joint, and a clicking sensation during knee movement.
What are the common causes of iliotibial band syndrome?
Common causes of ITBS include overuse from repetitive activities, biomechanical issues like poor alignment or weak hip muscles, and training errors such as sudden increases in mileage or intensity.
How prevalent is ITBS among athletes?
ITBS is particularly common among distance runners, with a reported incidence of 1.63% among race entrants.
What treatment options does RegenCore offer for ITB-related issues?
RegenCore offers innovative regenerative therapies, such as Platelet-Rich Plasma (PRP) injections and Bone Marrow Aspirate Concentrate (BMAC) treatments, to support recovery from ITB-related injuries.
What rehabilitation strategies can assist in managing ITB-related concerns?
Targeted rehabilitation strategies, including dynamic exercises and a calming period before active interventions, can help manage ITB-related concerns effectively.
List of Sources
- Understand the Iliotibial Band: Anatomy and Function
- Iliotibial band release significantly improves pain, function, and quality of life in patients with isolated patellofemoral osteoarthritis: A 2-year retrospective study – PubMed (https://pubmed.ncbi.nlm.nih.gov/41109608)
- Current Clinical Concepts: Synthesizing the Available Evidence for Improved Clinical Outcomes in Iliotibial Band Impingement Syndrome – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8359713)
- What’s New in Foot & Ankle? News to Know Before ACFAS 2026 (https://blog.smarttrak.com/whats-new-in-foot-ankle-news-to-know-before-acfas-2026)
- Research hotspots and current status of iliotibial band studies: A bibliometric analysis (1934–2023) – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12282822)
- Identify IT Band Syndrome: Symptoms and Causes
- hopkinsmedicine.org (https://hopkinsmedicine.org/health/conditions-and-diseases/iliotibial-band-syndrome)
- Risk factors associated with a history of iliotibial band syndrome (hITBS) in distance runners: a cross-sectional study in 76 654 race entrants – a SAFER XXXIII study – PubMed (https://pubmed.ncbi.nlm.nih.gov/38618688)
- Frontiers | Effects of conservative treatment strategies for iliotibial band syndrome on pain and function in runners: a systematic review (https://frontiersin.org/journals/sports-and-active-living/articles/10.3389/fspor.2024.1386456/full)
- Tightness and pain in leg could be due to IT band issues (https://uclahealth.org/news/article/tightness-and-pain-in-leg-could-be-due-to-it-band-issues)
- Diagnose IT Band Syndrome: Assessment Techniques
- my.clevelandclinic.org (https://my.clevelandclinic.org/health/diseases/21967-iliotibial-band-syndrome)
- An Investigation into the Iliotibial Band Assessment (IT Band Test) (https://burlingtonsportstherapy.com/blog/an-investigation-into-the-iliotibial-band-assessment-for-sports-related-pain)
- Evidence-Based Strategies for ITBS-Related Knee Pain (https://londoncartilage.com/insights/evidence-based-strategies-for-itbs-related-knee-pain)
- IT BAND SYNDROME- update on the current research (https://drdelanghe.com/it-band-syndrome-update-on-the-current-research)
- Iliotibial Band Syndrome (https://physio-pedia.com/Iliotibial_Band_Syndrome)
- Treat IT Band Syndrome: Effective Management Strategies
- princetonorthopaedic.com (https://princetonorthopaedic.com/it-band-syndrome-outer-knee-pain-and-treatment)
- Preventing and treating iliotibial (IT) band syndrome: Tips for pain-free movement – Harvard Health (https://health.harvard.edu/exercise-and-fitness/preventing-and-treating-iliotibial-it-band-syndrome-tips-for-pain-free-movement)
- Ground-breaking New Treatment for Iliotibial Band Syndrome (https://rtmslondon.com/iliotibial-band-syndrome)
- How to Avoid ITB Syndrome | EmergeOrtho-Foothills Region (https://emergeortho.com/news/how-to-avoid-itb-syndrome)
- Best Practices to Prevent and Treat IT Band Pain Effectively | RegenCore Method (https://regencoremethod.com/best-practices-to-prevent-and-treat-it-band-pain-effectively)
- Prevent IT Band Syndrome: Practical Tips for Active Professionals
- Iliotibial Band Syndrome: Prevention Tips and Early Intervention (https://search.mskdoctors.com/doctors/thomas-harrison/articles/iliotibial-band-syndrome-prevention-tips-and-early-intervention)
- Preventing and treating iliotibial (IT) band syndrome: Tips for pain-free movement – Harvard Health (https://health.harvard.edu/exercise-and-fitness/preventing-and-treating-iliotibial-it-band-syndrome-tips-for-pain-free-movement)
- Ground-breaking New Treatment for Iliotibial Band Syndrome (https://rtmslondon.com/iliotibial-band-syndrome)
- Manage Iliotibial Band Syndrome Hip Pain: 5 Essential Steps | RegenCore Method (https://regencoremethod.com/manage-iliotibial-band-syndrome-hip-pain-5-essential-steps)
- Tips for Runners on Managing IT Band Syndrome | UPMC (https://share.upmc.com/2024/06/prevent-it-band-injury)

