Introduction
Arthritis can weigh heavily on those it touches, often leaving them to wrestle with unrelenting pain and emotional turmoil. In the midst of this battle, arthritis biologics have emerged as a revolutionary class of treatments, thoughtfully designed to engage the immune system and reduce inflammation. As these therapies gain recognition, many find themselves wondering about their effectiveness, the science behind their action, and how they stand apart from traditional medications. What does the future hold for biologics in managing arthritis, and how might they transform the lives of those enduring chronic joint pain?
Define Arthritis Biologics: Understanding the Basics
Living with arthritis can feel overwhelming, as the pain and inflammation often disrupt daily life. For many, conditions like rheumatoid arthritis (RA) and osteoarthritis bring not just physical discomfort but emotional challenges too. The struggle to find relief can leave individuals feeling isolated and frustrated, yearning for relief and a return to normalcy.
Fortunately, there’s hope in the form of biologics, which are a specialized class of medications derived from living organisms. These medications are designed to specifically target components of the immune system, working to reduce inflammation and prevent joint damage. Unlike conventional medications that are chemically synthesized, biologics harness the power of biological processes involving cells or tissues. This unique approach allows them to effectively inhibit specific pathways in the immune response, alleviating symptoms and slowing disease progression.
Among the most promising examples of biologics are tumor necrosis factor (TNF) inhibitors and interleukin inhibitors. They have truly transformed the landscape of joint disorder care, offering targeted options that can lead to significant improvements. Imagine experiencing a noticeable decrease in discomfort and enhanced mobility—this is the reality for many who have turned to biologics. Research shows that these therapies can greatly improve the quality of life for patients, helping them reclaim their daily activities and joy.
Looking ahead to 2026, it’s anticipated that more individuals will embrace biological therapies for arthritis. This growing acceptance reflects not only their efficacy but also a shift towards more compassionate care in managing chronic conditions. With these advancements, there’s a renewed sense of hope for those battling arthritis, reminding us that relief is possible and that no one has to face this journey alone.
Contextualize Biologics: Their Role in Arthritis Management
For many individuals battling joint inflammation, the journey can feel overwhelming, especially when conventional disease-modifying antirheumatic drugs (DMARDs) fail to provide the relief they desperately seek. At RegenCore, we understand the emotional toll this struggle takes. Our innovative therapies harness naturally derived cell-based substances and a variety of regenerative modalities, offering a personalized approach to healing arthritic or injured joints. This not only enhances recovery but also works to reverse damage, providing hope where it may have seemed lost.
This is particularly crucial for those grappling with moderate to severe arthritis, where unchecked inflammation can lead to joint damage. Imagine living with constant pain and swelling, feeling as though your body is betraying you. Our biologics specifically target inflammation, alleviating these distressing symptoms while also improving overall function and quality of life. This shift in care paradigms has paved the way for more effective treatments, tailored to meet the unique needs of each patient.
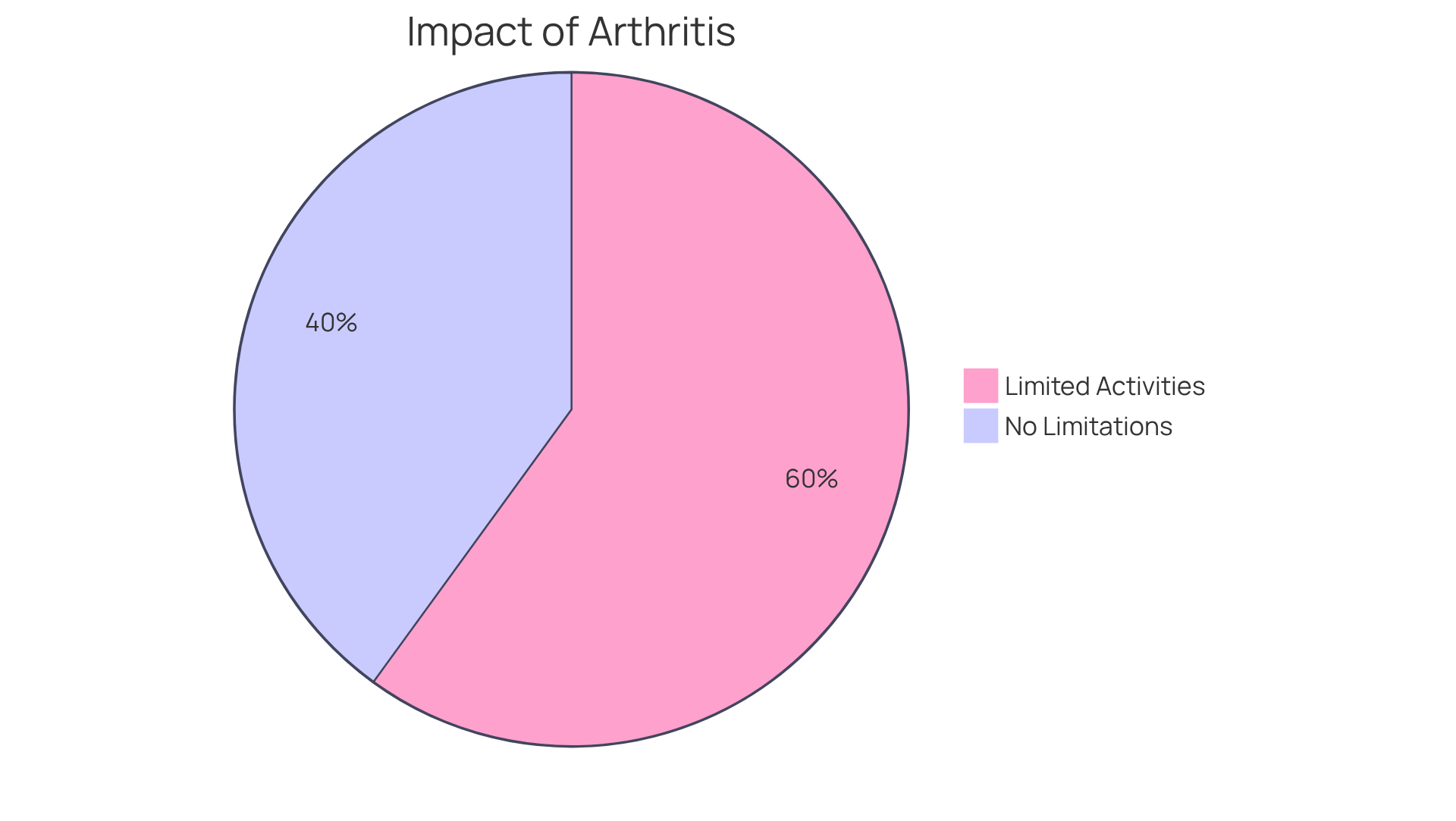
Statistics reveal a staggering reality: around 60% of working-age adults with arthritis face limitations in their daily activities due to their condition. This underscores the urgent need for effective therapies. The introduction of biologics has truly transformed the field of rheumatology, providing innovative solutions that were once out of reach for those enduring chronic pain. As experts continue to explore the effectiveness of these therapies, their role in enhancing patient outcomes remains a vital aspect of modern joint disease management, bringing renewed hope and a brighter future for many.
Trace the Evolution: The Development of Biologics in Medicine
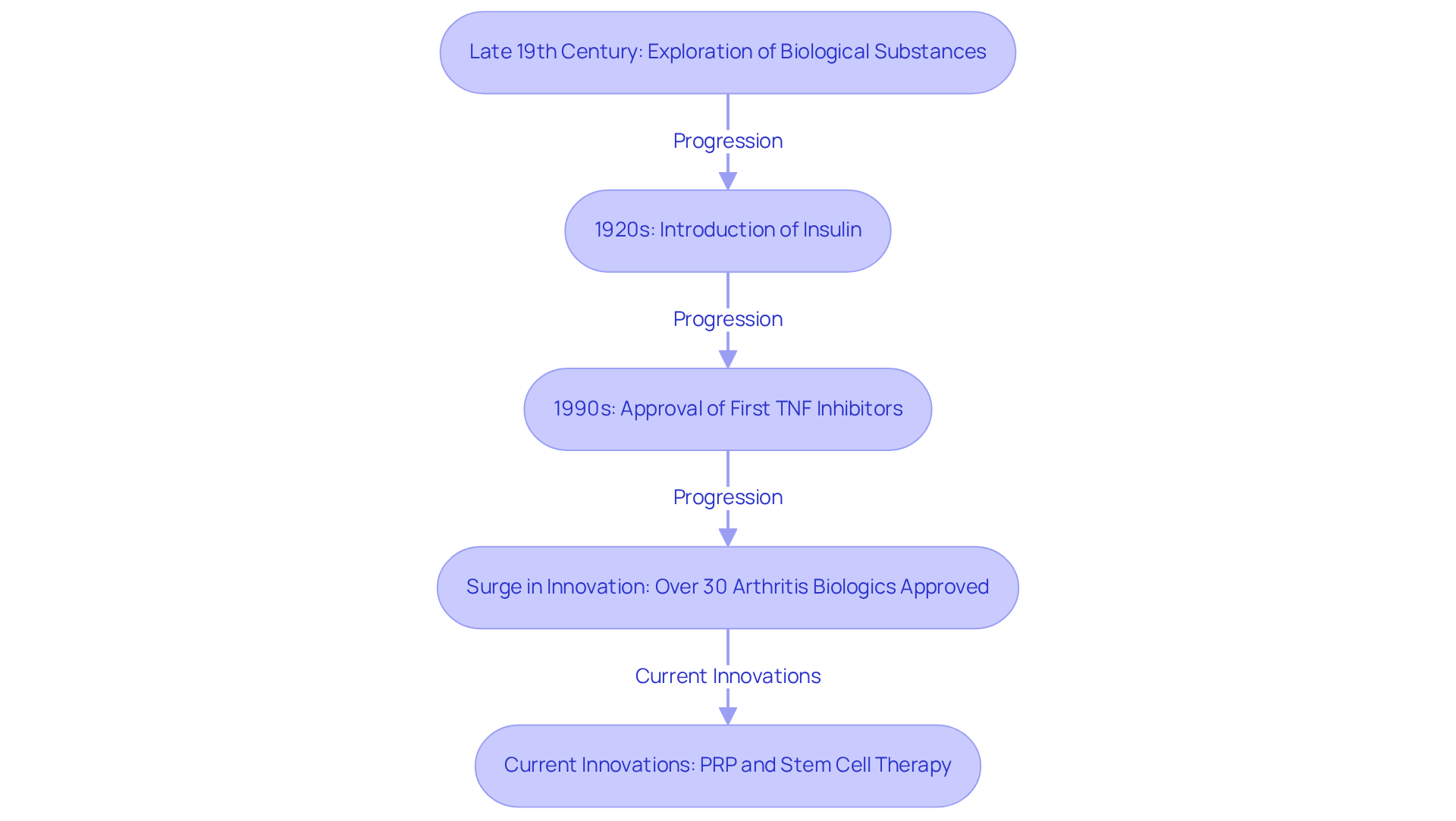
The journey of biological medicines in healthcare began in the late 19th century, as dedicated researchers explored the healing potential of biological substances. A significant milestone was reached in the 1920s with the introduction of insulin, a breakthrough that paved the way for future advancements in biologics. Fast forward to the 1990s, a transformative era emerged with the approval of the first TNF inhibitors, which dramatically changed the management of autoimmune diseases, especially through the use of biologic therapies. This period marked a surge in innovation, leading to over 30 arthritis biologics being approved for various arthritic conditions, reflecting a revolution in biotechnology.
These advancements have not only led to the creation of more treatment options but have also significantly improved patient outcomes, particularly in pain management. At RegenCore, we understand the emotional and physical toll that conditions like arthritis can take on individuals. That’s why we’re committed to taking this evolution a step further by offering personalized therapies that harness the power of naturally derived cell-based biologics.
Our services, including:
are thoughtfully designed to enhance healing and promote recovery in arthritic or injured joints. We believe in providing a solution that aligns with the latest advancements in biologic medicine, ensuring that each patient receives the compassionate care they deserve on their journey to recovery.
Explore Mechanisms: How Biologics Work in Treating Arthritis
Living with arthritis can be a daily struggle, as it often leads to pain and limited mobility. Many patients find themselves grappling with the frustration of not being able to enjoy life fully due to this relentless condition. It’s a challenge that can feel isolating, but biologics can offer hope.
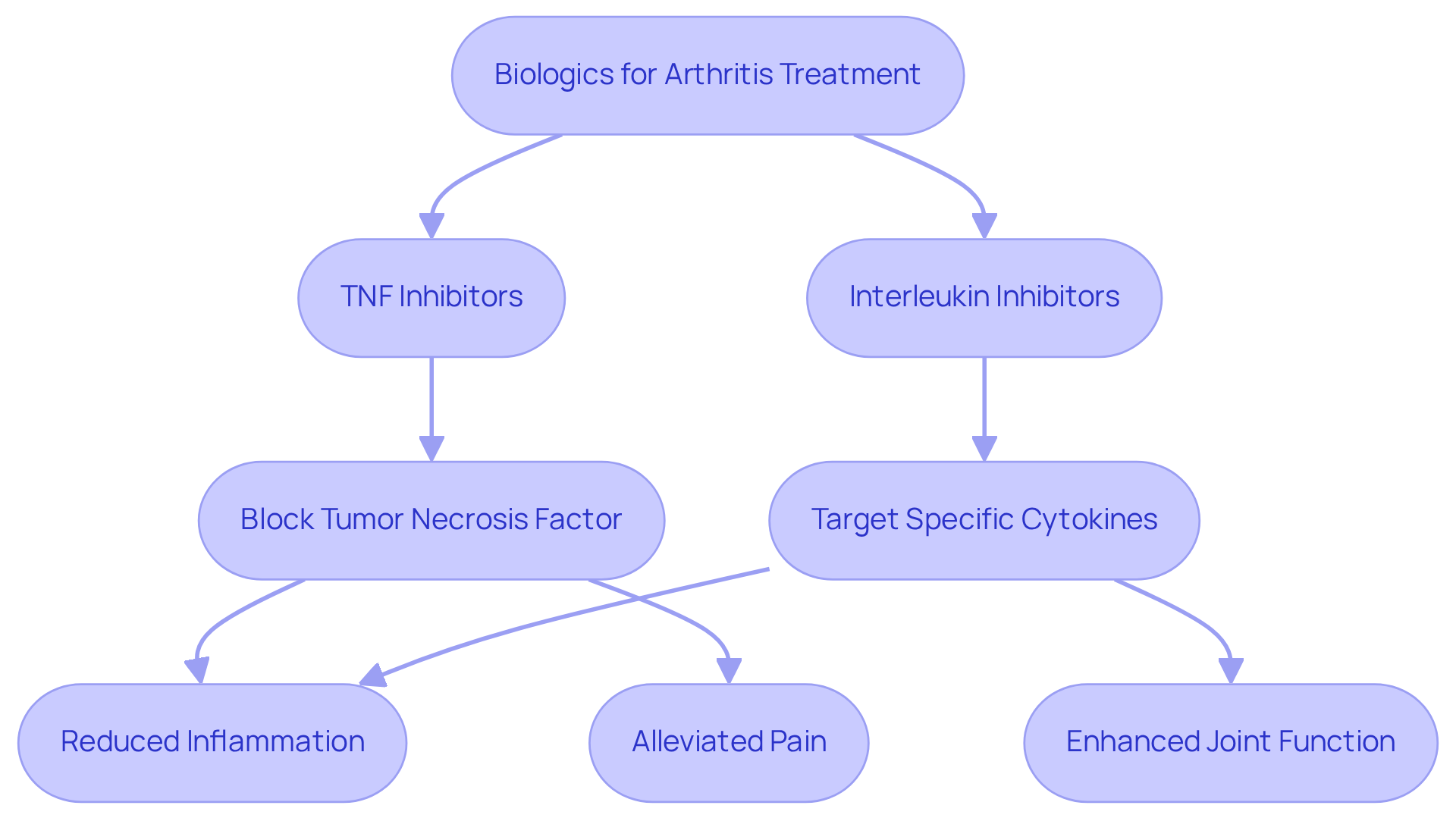
Biologics have emerged as a beacon of hope for individuals suffering from arthritis. These innovative therapies are designed to target factors that contribute to the inflammatory process. For instance, TNF inhibitors work by blocking tumor necrosis factor, a cytokine that plays a crucial role in driving inflammation. By inhibiting this pathway, these therapies can significantly reduce symptoms, alleviating pain and enhancing mobility. Imagine waking up each day with less pain and more freedom to move—this is the promise that biologics hold.
Similarly, interleukin inhibitors focus on different cytokines within the inflammatory cascade, providing a targeted approach that can lead to more effective symptom management. For many patients, this means not just relief but also the ability to engage in daily activities. It’s about reclaiming a life that arthritis has overshadowed.
Understanding these mechanisms is vital for healthcare professionals, as it allows them to develop treatment plans that truly resonate with their patients’ needs. It also empowers individuals to grasp the reasoning behind their therapies, fostering a sense of control in their treatment journey. The practical applications of biologics have demonstrated encouraging results, with numerous patients experiencing significant improvements. These innovative therapies are not just treatments; they represent a path toward a brighter, more active future.
Identify Examples: Common Biologics Used for Arthritis
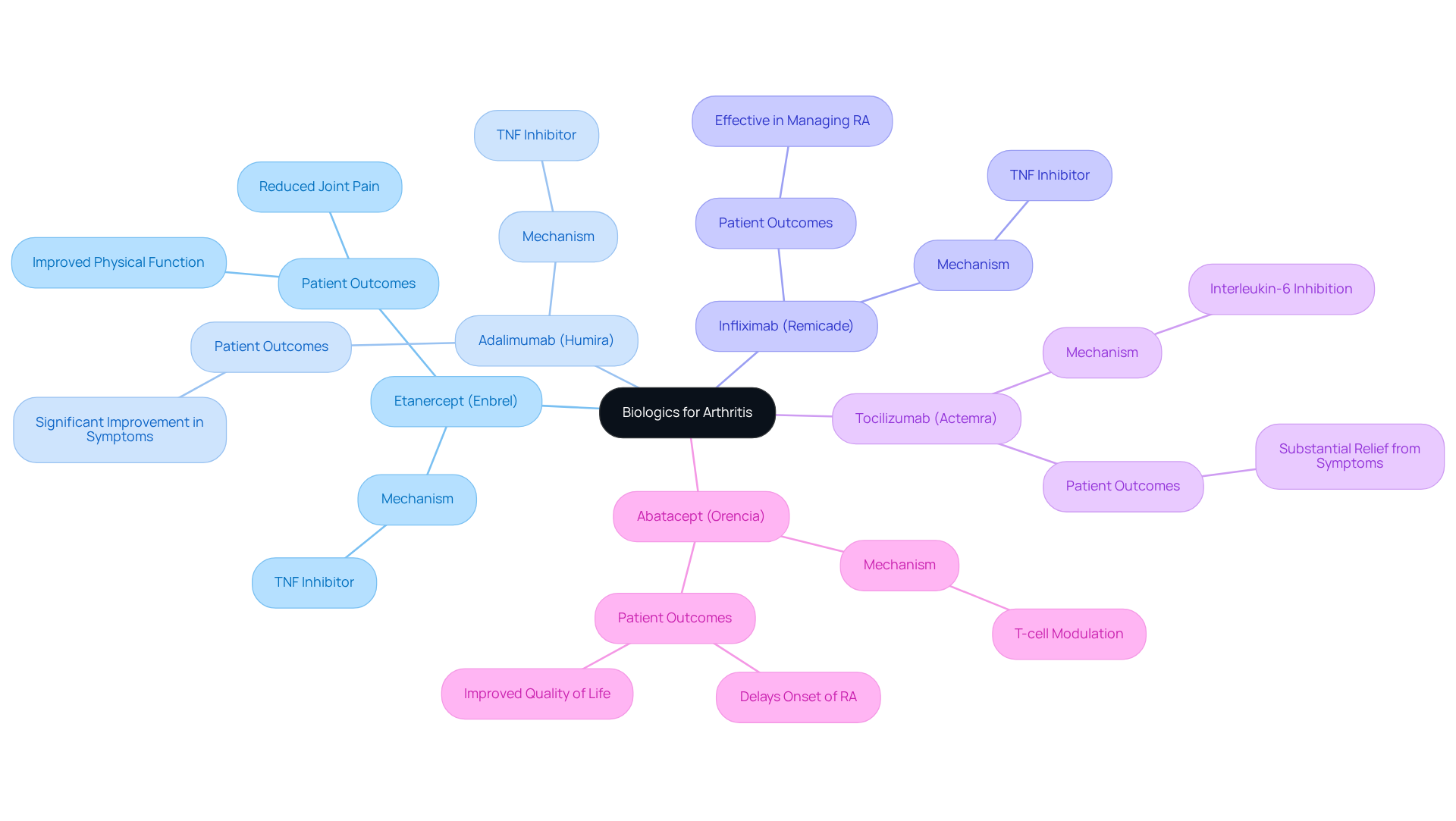
Living with arthritis can be a daily struggle, affecting not just physical health but emotional well-being too. Many individuals find themselves battling persistent pain and reduced mobility, which can lead to feelings of frustration and helplessness. Common biologics, such as etanercept (Enbrel), adalimumab (Humira), and infliximab (Remicade), offer hope by functioning as TNF inhibitors that effectively reduce inflammation by blocking tumor necrosis factor, a key player in inflammatory processes. These treatments have transformed lives, but the journey to finding the right solution can be overwhelming.
Imagine waking up each day, hoping for relief, only to be met with the same discomfort. Infliximab, a chimeric monoclonal antibody, also targets TNF, providing another avenue for managing rheumatoid arthritis and other autoimmune diseases. The emotional toll of living with such conditions is profound, and it’s crucial to understand that you’re not alone in this fight. Additionally, tocilizumab (Actemra) inhibits interleukin-6, while abatacept (Orencia) modulates T-cell activation, which enhances the effectiveness of treatment strategies. Studies have consistently shown the effectiveness of biologics, which has led to their widespread adoption in clinical practice.
For many, the results have been life-changing. Etanercept and adalimumab have shown significant improvements in patient-reported outcomes, including reduced joint pain and enhanced physical function. Real-world experiences with tocilizumab and abatacept further underscore their effectiveness, with countless individuals reporting substantial relief from symptoms. Understanding biologics empowers both patients and healthcare professionals to make informed choices about care alternatives, ultimately improving the management of arthritis.
At RegenCore, we recognize the challenges you face and enhance these conventional approaches with innovative therapies. Our innovative methods utilize naturally derived cell-based biologics to promote healing and reverse tissue damage. We offer a comprehensive treatment plan, providing patients with additional choices for managing their conditions. Ongoing research is also exploring new therapies, bringing hope for improved outcomes in the future. Together, we can navigate this journey towards better health and well-being.
Clarify Related Concepts: Biologics vs. Biosimilars
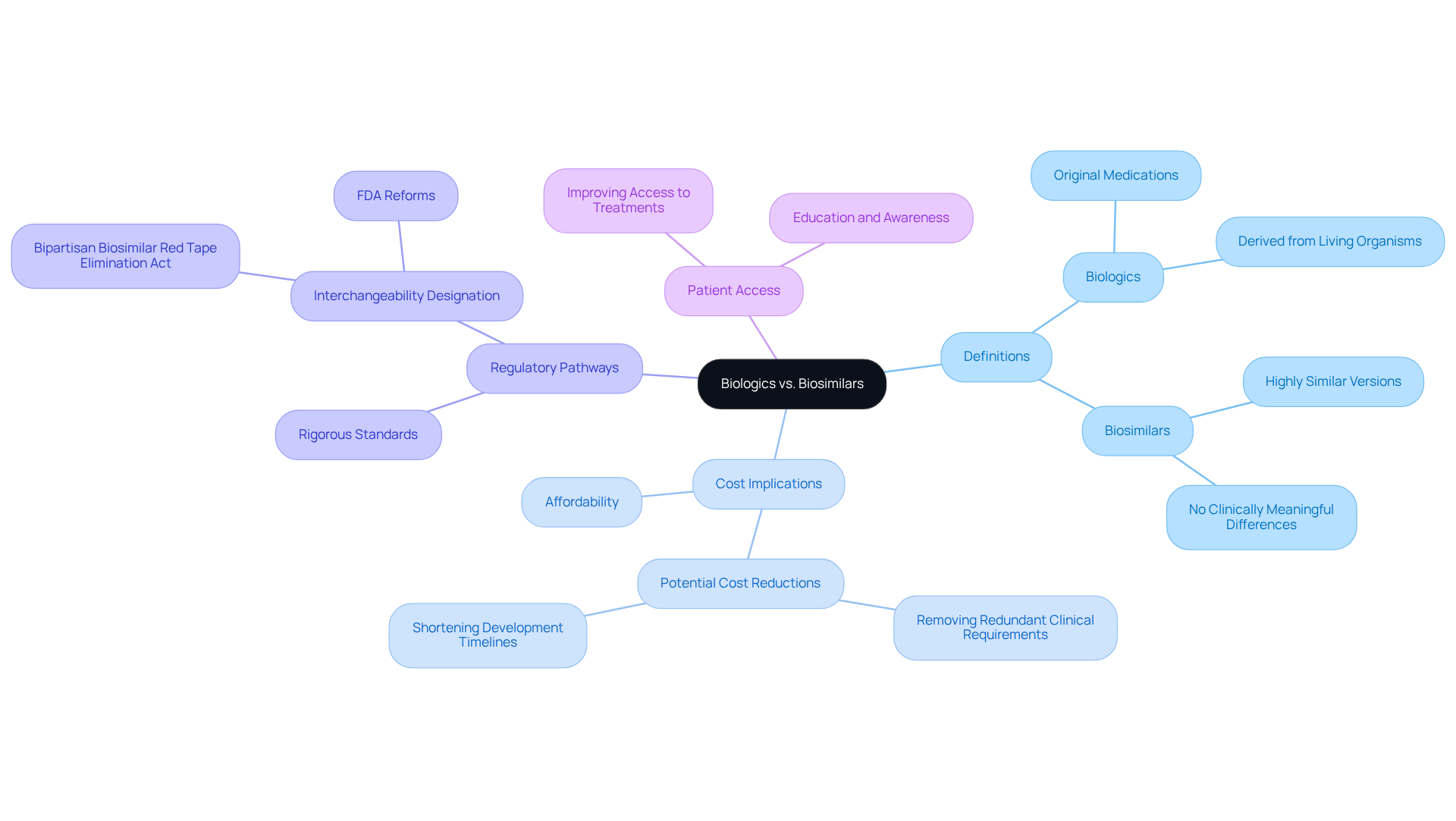
While arthritis biologics and biosimilars often create confusion, they play crucial roles in treating conditions like arthritis. For many patients, the high costs of biologics can feel overwhelming, leaving them anxious about their treatment options. Biologics are original medications derived from living organisms, specifically designed to target the pathways involved in disease processes. On the other hand, biosimilars are highly similar versions of these biological products, showing no clinically meaningful differences in safety and efficacy. This distinction is vital, as it directly impacts patients’ treatment choices.
The introduction of biosimilars offers a beacon of hope for those managing arthritis. While biologics can be prohibitively expensive, biosimilars present a more affordable alternative, making it easier for individuals to access the treatments they need. Imagine the relief of knowing that effective therapies are within reach, without the burden of exorbitant costs. Analysts suggest that by removing redundant clinical requirements, development costs for biosimilars could drop by tens of millions of dollars per product, further reinforcing their potential to improve patient access.
Biosimilars maintain quality and performance, which is essential for their integration into treatment plans. As Alex Keeton, Executive Director of the Biosimilars Council, expressed, “This reform would help ensure lower-cost biosimilars can be substituted at the pharmacy counter, improving access across the country.” This reform is significant, as it shapes healthcare policies, influences costs, and ultimately affects the accessibility of vital therapies. By embracing biosimilars, we can foster a more compassionate healthcare landscape, where every patient has the opportunity to receive the care they deserve.
Conclusion
The landscape of arthritis treatment is changing, and for many, biologics are becoming a beacon of hope. These groundbreaking therapies, derived from living organisms, specifically target the inflammatory pathways that cause so much pain and discomfort. Unlike traditional medications, which often provide only temporary relief, biologics offer a more personalized approach, addressing the unique needs of each patient. As more individuals seek out these treatments, the potential for improved symptom management and a better quality of life becomes clearer.
Throughout this discussion, we see the profound impact biologics can have on managing arthritis. From their historical development to the specific ways they work, understanding these therapies is crucial for anyone affected by this condition. The introduction of various biologics, such as TNF inhibitors and interleukin inhibitors, showcases their effectiveness in alleviating pain and enhancing patient outcomes. Moreover, distinguishing between biologics and biosimilars highlights the importance of having accessible treatment options in a compassionate healthcare environment.
Given these advancements, it’s essential for both patients and healthcare providers to stay updated on the latest in arthritis biologics. Embracing these therapies not only brings hope but also empowers individuals to take back control of their lives from the clutches of arthritis. As research continues to reveal new possibilities in the world of biologics, the future shines bright for those yearning for relief from chronic joint inflammation.
Frequently Asked Questions
What are arthritis biologics?
Arthritis biologics are specialized medications derived from living organisms that specifically target components of the immune system to reduce inflammation and prevent joint damage in conditions like rheumatoid arthritis (RA) and osteoarthritis.
How do arthritis biologics differ from conventional medications?
Unlike conventional medications that are chemically synthesized, arthritis biologics utilize biological processes involving cells or tissues, allowing them to effectively inhibit specific pathways in the immune response.
What are some examples of arthritis biologics?
Some promising examples of arthritis biologics include tumor necrosis factor (TNF) inhibitors and interleukin inhibitors, which have transformed the care landscape for joint disorders.
What benefits do arthritis biologics offer to patients?
Arthritis biologics can lead to significant improvements in symptoms, such as decreased discomfort and enhanced mobility, greatly improving the quality of life for individuals with arthritis.
What is the expected trend for the use of biological therapies by 2026?
It is anticipated that more individuals will embrace biological therapies for joint inflammation treatment by 2026, reflecting their efficacy and a shift towards more compassionate care in managing chronic issues.
How do biologics play a role in arthritis management?
Biologics target inflammatory pathways, alleviating distressing symptoms and improving overall function and quality of life, particularly for those with moderate to severe arthritis where unchecked inflammation can cause irreversible joint damage.
What is the impact of arthritis on daily activities?
Statistics show that around 60% of working-age adults with joint pain face limitations in their daily activities due to their condition, highlighting the urgent need for effective treatment options.
How have arthritis biologics transformed the field of rheumatology?
The introduction of arthritis biologics has provided innovative solutions for chronic inflammatory conditions, enhancing patient outcomes and offering renewed hope for many individuals battling joint inflammation.
List of Sources
- Define Arthritis Biologics: Understanding the Basics
- Study identifies alternate path for inflammation that could improve RA treatment (https://news.wsu.edu/press-release/2026/01/30/study-identifies-alternate-path-for-inflammation-that-could-improve-ra-treatment)
- Biologics (https://arthritis.org/drug-guide/biologics/biologics)
- Organogenesis Holdings Inc. Initiates Biologics License Application for ReNu® to Address Knee Osteoarthritis Pain | ORGO Stock News (https://quiverquant.com/news/Organogenesis+Holdings+Inc.+Initiates+Biologics+License+Application+for+ReNu®+to+Address+Knee+Osteoarthritis+Pain)
- The 2026 Biologics Wave: Which Innovations Will Break Through? (https://contractpharma.com/the-2026-biologics-wave-which-innovations-will-break-through)
- Contextualize Biologics: Their Role in Arthritis Management
- Biologic DMARDs Improve Clinical Response Outcomes in Polyarticular JIA (https://rheumatologyadvisor.com/news/bdmards-vs-standard-therapy-improve-clinical-responses-in-pjia)
- Breakthrough Therapies Offering New Hope for Millions (https://americanarthritisfoundation.org/b/breakthrough-therapies-offering-new-hope-for-millions)
- Advance Treatment Can Delay Onset Of Rheumatoid Arthritis By Years, Trial Data Show (https://usnews.com/news/health-news/articles/2026-01-22/advance-treatment-can-delay-onset-of-rheumatoid-arthritis-by-years-trial-data-show)
- The 2026 Biologics Wave: Which Innovations Will Break Through? (https://contractpharma.com/the-2026-biologics-wave-which-innovations-will-break-through)
- Prescription Arthritis Medications Market Outlook 2026-2034 (https://intelmarketresearch.com/prescription-arthritis-medications-market-34818)
- Trace the Evolution: The Development of Biologics in Medicine
- Breakthrough Therapies Offering New Hope for Millions (https://americanarthritisfoundation.org/b/breakthrough-therapies-offering-new-hope-for-millions)
- How New Therapies Are Revolutionizing the Treatment of Juvenile Idiopathic Arthritis (https://rutgershealth.org/news/how-new-therapies-are-revolutionizing-treatment-juvenile-idiopathic-arthritis)
- Innovative Biologics – Expected Biologic Drug Approvals in 2026 (https://mabion.eu/science-hub/articles/innovative-biologics-expected-approvals-in-2026)
- FDA OKs a New Biologic for RA (https://arthritis.org/news/fda-approves-new-rheumatoid-arthritis-biologic-sar)
- Explore Mechanisms: How Biologics Work in Treating Arthritis
- Challenge accepted: UCLA Health team works at warp speed to defeat osteoarthritis (https://uclahealth.org/news/article/challenge-accepted-ucla-health-team-works-warp-speed-defeat)
- Early treatment can delay rheumatoid arthritis for years (https://medicalxpress.com/news/2026-01-early-treatment-delay-rheumatoid-arthritis.html)
- From Breakthrough to Everyday Treatment: Biologics Revolutionizing Inflammatory Disease Management (https://iqone-healthcare.com/news/biologics)
- Breakthrough Therapies Offering New Hope for Millions (https://americanarthritisfoundation.org/b/breakthrough-therapies-offering-new-hope-for-millions)
- Identify Examples: Common Biologics Used for Arthritis
- Advance Treatment Can Delay Onset Of Rheumatoid Arthritis By Years, Trial Data Show (https://healthday.com/health-news/bone-and-joint/advance-treatment-can-delay-onset-of-rheumatoid-arthritis-by-years-trial-data-show)
- New Therapies for Rheumatoid Arthritis Pain (https://verywellhealth.com/new-rheumatoid-arthritis-treatment-5221441)
- Advance Treatment Can Delay Onset Of Rheumatoid Arthritis By Years Trial Data Show (https://powershealth.org/about-us/newsroom/health-library/2026/01/22/advance-treatment-can-delay-onset-of-rheumatoid-arthritis-by-years-trial-data-show)
- Early treatment can delay rheumatoid arthritis for years (https://medicalxpress.com/news/2026-01-early-treatment-delay-rheumatoid-arthritis.html)
- Clarify Related Concepts: Biologics vs. Biosimilars
- Biosimilars: expanding access to essential biologic therapies (https://who.int/news/item/13-02-2025-biosimilars–expanding-access-to-essential-biologic-therapies)
- FDA Draft Guidance on Biosimilars Is a Win for Patients; Now Congress Must Finish the Job (https://centerforbiosimilars.com/view/fda-draft-guidance-on-biosimilars-is-a-win-for-patients-now-congress-must-finish-the-job)
- FDA Moves to Accelerate Biosimilar Development and Lower Drug Costs (https://fda.gov/news-events/press-announcements/fda-moves-accelerate-biosimilar-development-and-lower-drug-costs)

