Introduction
Understanding the complexities of iliotibial band syndrome (ITBS) reveals not just the physical challenges it brings, but also the emotional toll it can take on overall well-being. This common overuse injury often manifests as discomfort along the outer knee, leaving many individuals wondering if it could also lead to lower back pain. Research suggests a significant connection, highlighting how the tightness and dysfunction of the IT band can disrupt biomechanics and strain the lumbar spine. This intertwining of issues can feel overwhelming, but there are strategies to address them. By exploring these connections, we can work towards restoring balance to both the knee and back, offering hope and relief to those affected.
Define IT Band Syndrome: Understanding the Condition
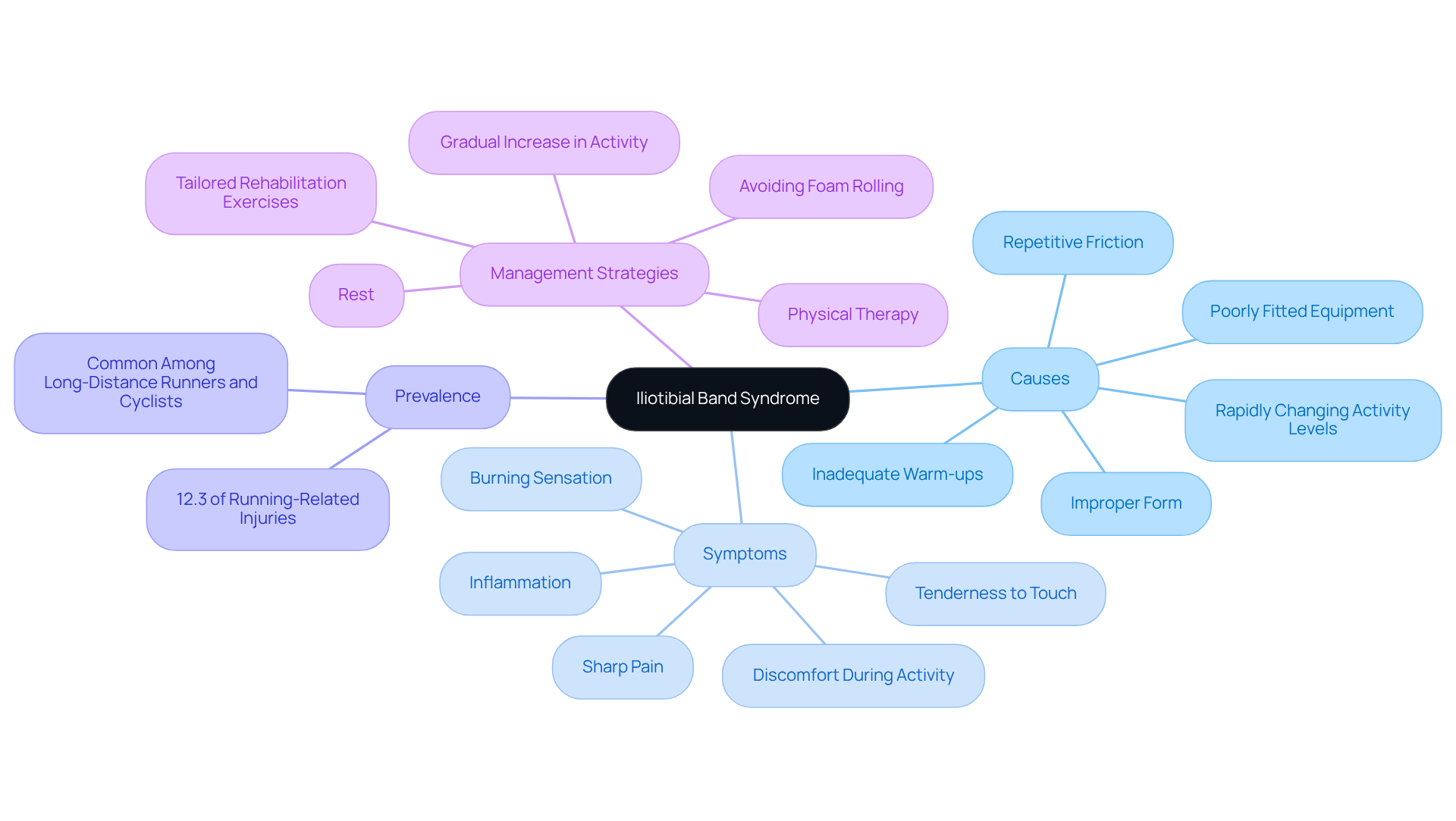
can be a frustrating overuse injury, often leaving individuals with discomfort and inflammation along the iliotibial band, that strong band of tissue stretching from the hip to the knee. For many, this condition emerges from the repetitive friction of the IT band against the lateral femoral condyle during activities like running, cycling, or hiking. Imagine feeling a sharp or burning pain on the outer side of your knee, especially when you’re trying to enjoy a run or even just sitting for a while with bent knees. It’s a struggle that can intensify with activity, particularly during downhill running.
Research shows that IT Band Syndrome accounts for about 12% of all running injuries, highlighting how common it is among athletes, especially runners and cyclists. It’s easy to see how improper form or equipment can exacerbate this issue, making it all the more important to address. Experts emphasize that if this condition isn’t fully addressed prior to returning to activity, it can become a chronic issue, which is why prevention is crucial.
Effective management often involves:
- Rest
- Tailored rehabilitation exercises designed to strengthen the hip and improve flexibility
At RegenCore, we understand the challenges you face, and we offer personalized treatment plans to promote healing and reverse tissue damage. Our approach is custom-tailored to support your recovery, backed by research that demonstrates both safety and efficacy in addressing the root causes of IT Band Syndrome.
It’s also important to recognize that therapies like foam rolling and massage may not be effective for this condition due to the unique characteristics of the IT band. Additionally, factors such as rapidly changing activity levels and inadequate warm-ups can contribute to the onset of this frustrating issue. By understanding the key characteristics and symptoms of IT Band Syndrome, athletes and active individuals can take proactive steps to prevent and address it, ultimately enhancing their performance and quality of life.
Explore the Link: IT Band Syndrome and Lower Back Pain
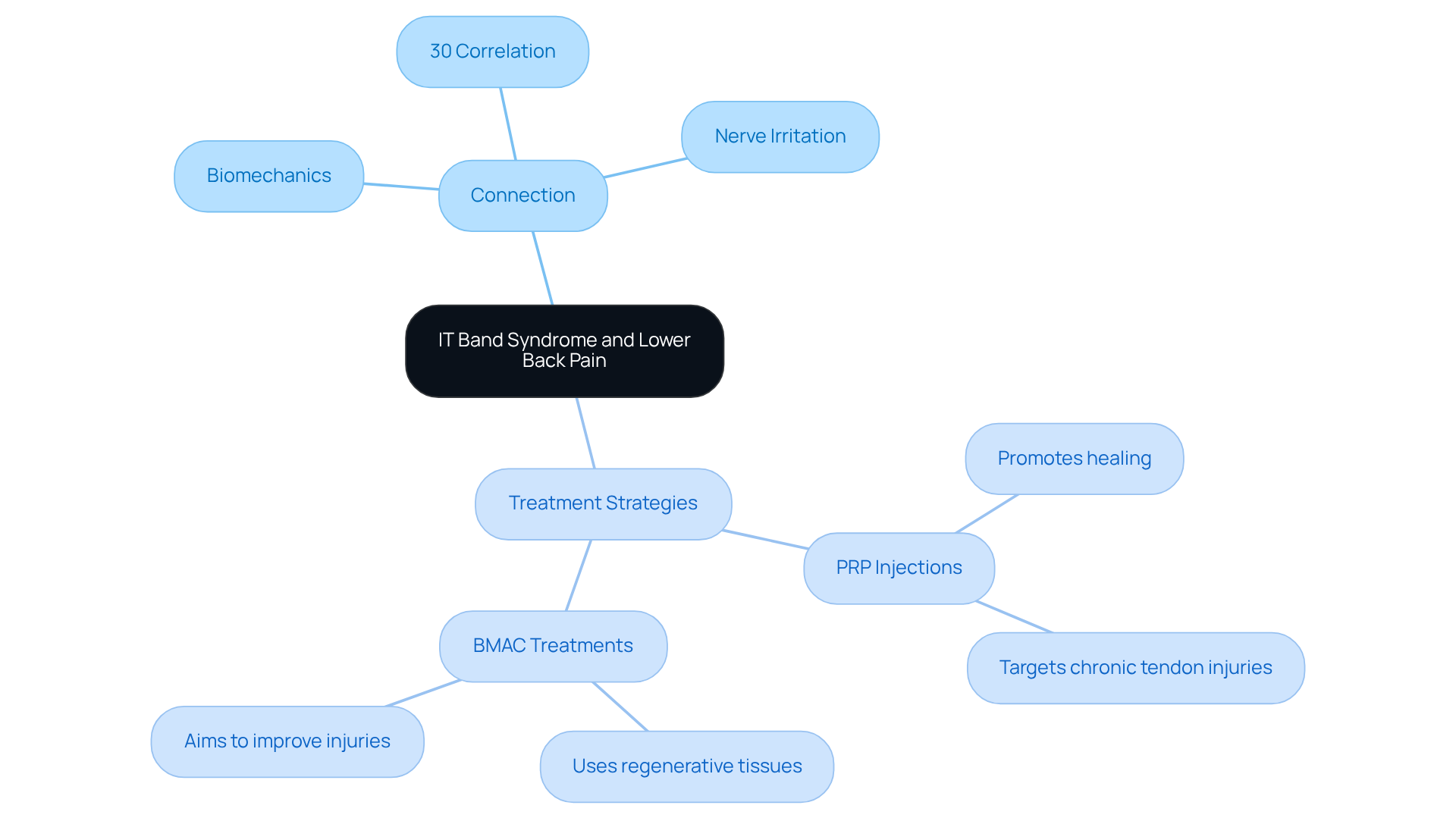
Recent studies reveal that many individuals question whether IT Band Syndrome can cause lower back pain, highlighting a significant connection between the two. The iliotibial band can become tight or dysfunctional, leading to altered biomechanics that may place undue stress on the lumbar spine. Imagine dealing with inadequate alignment or muscle imbalances in your lower back, only to find that these issues exacerbate your symptoms, creating a frustrating cycle of discomfort. Research shows that about 30% of those with IT Band Syndrome experience lower back pain, highlighting the intertwined nature of these conditions. Furthermore, irritation of lumbar nerves can weaken the muscles that support the IT band, complicating recovery even more.
At RegenCore, we truly understand the significance of this relationship. We’re committed to developing comprehensive treatment plans that address both IT Band Syndrome and the question of whether it can cause lower back pain. Our innovative therapies harness the body’s natural healing process, delivering platelets and growth factors directly into the injured area. This promotes repair for sprained or degenerated knees and hips. Similarly, our treatments involve injecting corticosteroids, aimed at improving injuries and conditions affecting tendons, ligaments, and joints. These therapies empower you to move pain-free, ensuring that active professionals can return to their routines without discomfort.
Identify Causes: Factors Leading to IT Band Syndrome
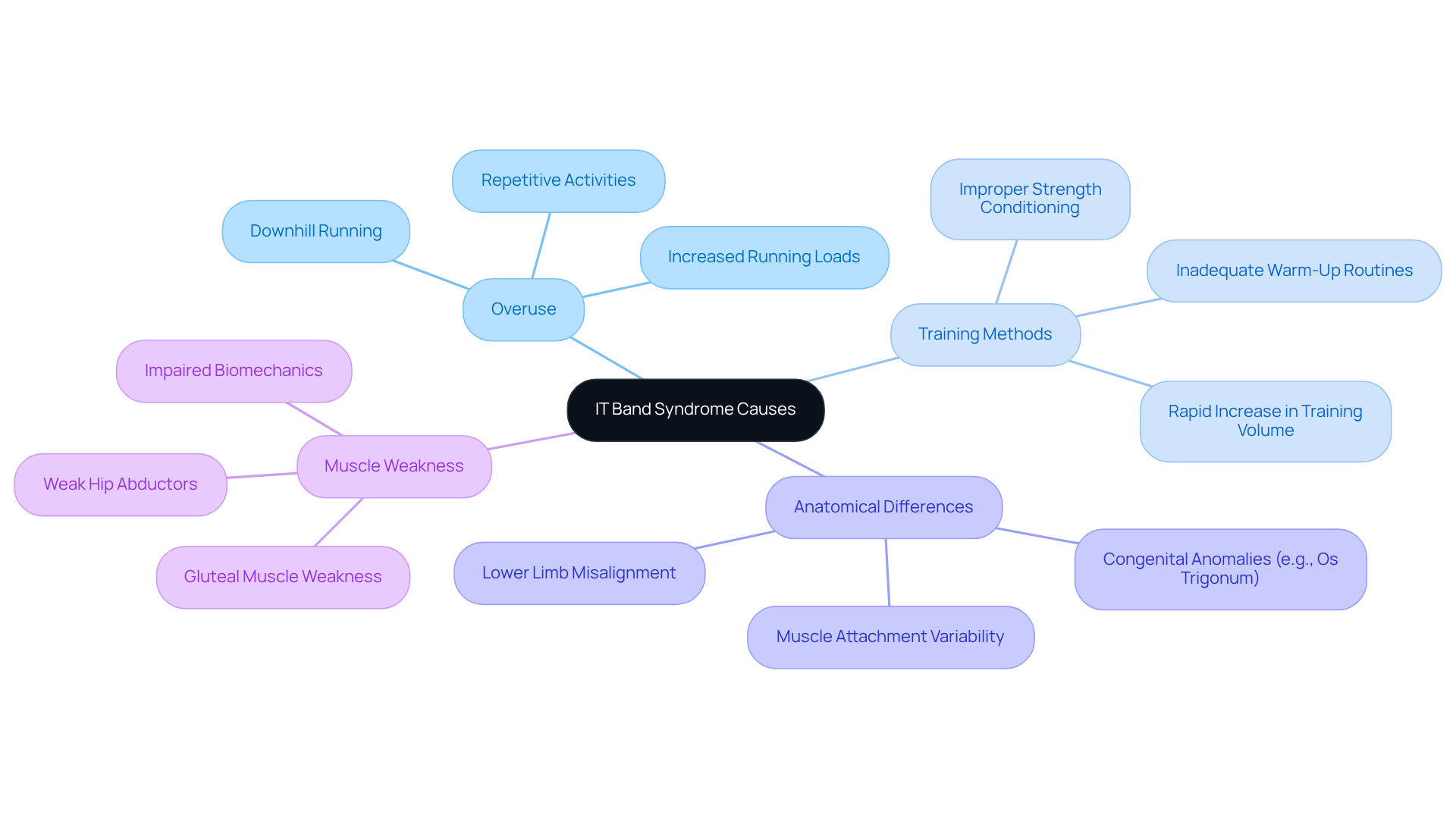
can be a frustrating and painful experience, often stemming from a mix of factors like overuse, inadequate training methods, and even anatomical differences. For many, running especially on uneven surfaces can lead to this condition. It’s not just about the activity itself; weakness in the muscles can disrupt biomechanics, increasing the likelihood of developing pain.
Imagine the disappointment of a runner who suddenly finds themselves sidelined due to pain. Tightness in the iliotibial band and surrounding muscles can worsen friction and inflammation, making every step feel like a struggle. For instance, runners who ramp up their mileage too quickly without proper strength conditioning often find themselves more susceptible to this injury. Recognizing these underlying causes is essential for athletes and active individuals alike. It empowers them to take proactive steps in preventing this condition and adjusting their training methods effectively.
Coaches and trainers play a vital role in this journey, emphasizing the importance of strength training and proper warm-up routines. They advocate for a holistic approach to training that considers both physical conditioning and biomechanics. By fostering an understanding of these elements, athletes can not only mitigate the risk of injury but also enhance their overall performance and well-being.
Recognize Symptoms: Signs of IT Band Syndrome
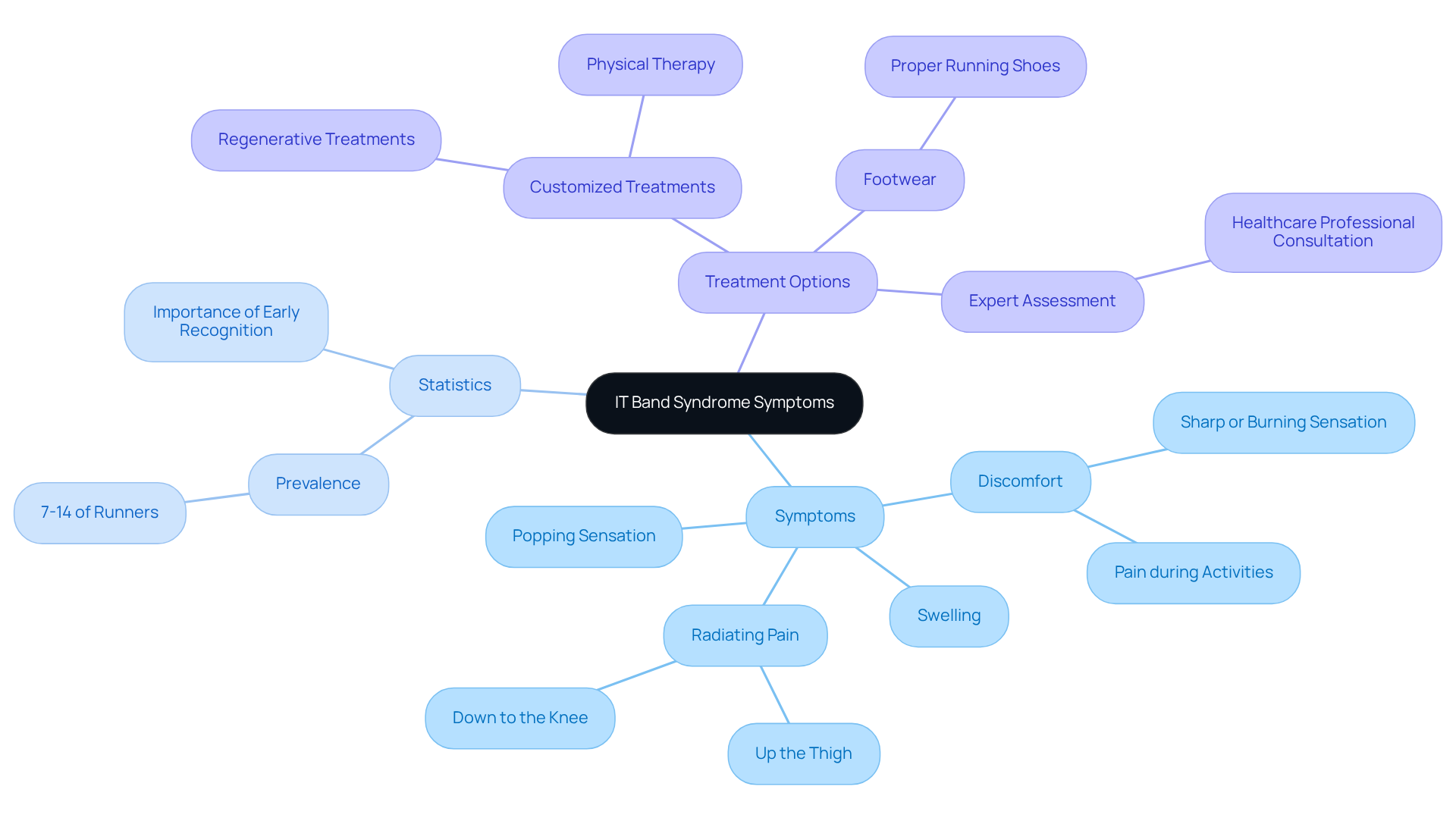
Experiencing discomfort on the outer side of the knee can be incredibly frustrating. Many patients describe this sensation as sharp or burning, especially during activities like running or climbing stairs. Along with this discomfort, swelling and sensitivity often accompany the pain, making even simple movements feel daunting. Some may even notice a popping sensation when moving their knee or hip, with discomfort radiating up the thigh or down to the knee. Early intervention is crucial for recovery.
Research indicates that 7-14% of runners face IT Band Syndrome, highlighting how common this condition is among athletes. This statistic can feel overwhelming, but it’s important to remember that early recognition can significantly improve treatment outcomes. When symptoms are caught early, appropriate interventions can alleviate pain and prevent further complications. For instance, one patient who recognized their symptoms early was able to run at RegenCore. This story underscores the importance of being aware of your body and taking prompt action.
At RegenCore, we offer customized treatment plans that are both safe and effective. Our approach utilizes naturally sourced cell-based biologics to enhance healing and support recovery from injuries, including IT Band Syndrome. It’s essential to interact with healthcare experts for a comprehensive assessment, as they can help differentiate IT Band Syndrome from other conditions, ensuring that the right treatment approaches are applied.
Moreover, wearing suitable footwear plays a vital role in preventing IT-related issues. Specific physical examination findings, such as point tenderness at the lateral femoral epicondyle, can also provide valuable diagnostic context. Remember, you’re not alone in this journey, and with the right support and awareness, recovery is within reach.
Discuss Treatment Options: Managing IT Band Syndrome
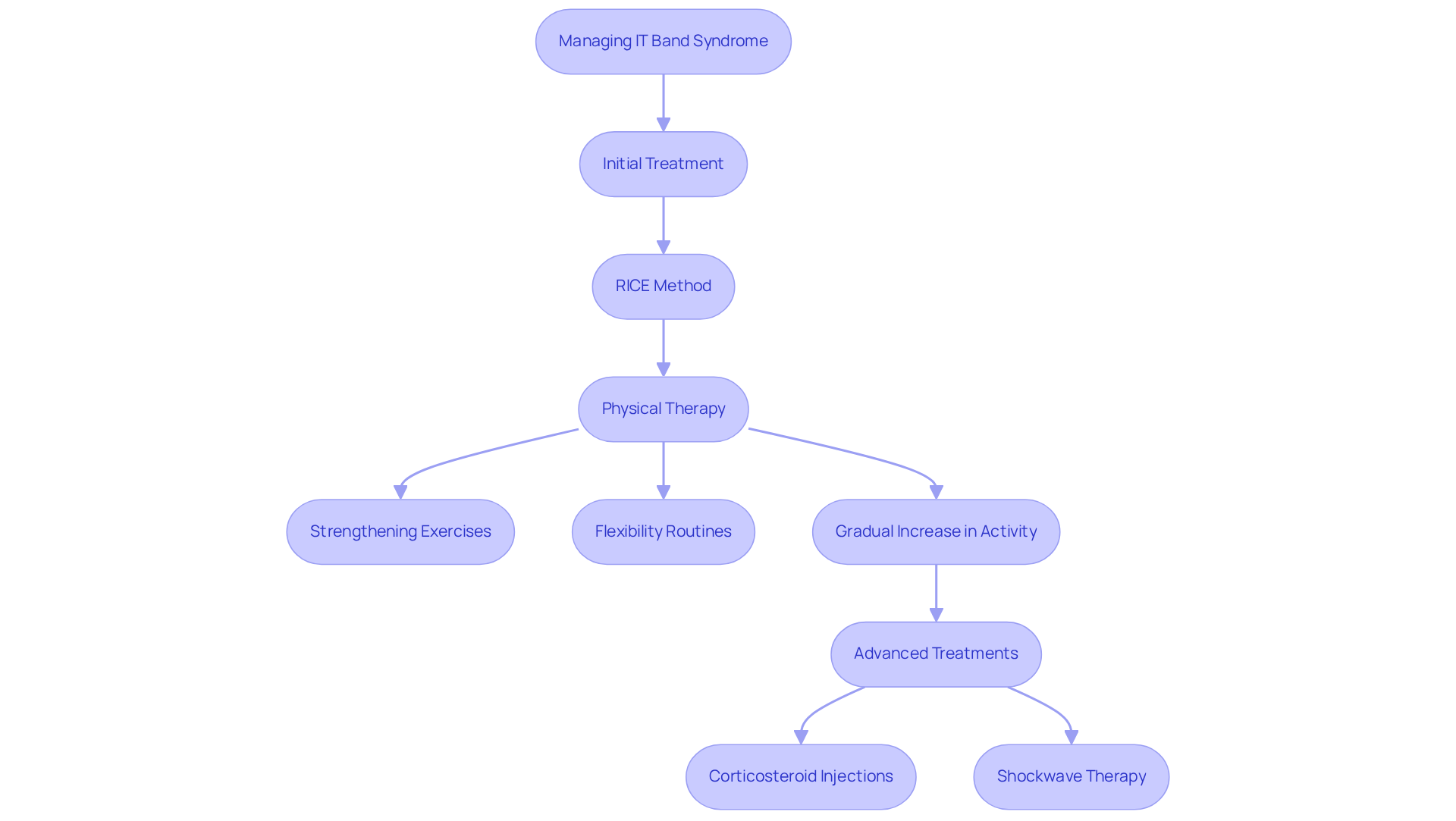
Dealing with IT Band Syndrome and understanding the condition can feel overwhelming, but you’re not alone in this journey. Many people struggle with the pain and limitations it brings, leading them to wonder about effective solutions, which makes everyday activities a challenge. The good news is that managing this condition effectively involves a multifaceted approach that includes rest, physical therapy, and thoughtful adjustments to your activity levels. In the beginning, the use of ice can be a lifeline, helping to reduce inflammation and ease your discomfort.
Physical therapy is a cornerstone of recovery, focusing on strengthening your hip and gluteal muscles while enhancing flexibility. It’s important to address the underlying issues that might be contributing to your pain, such as muscle imbalances. Imagine incorporating specific stretching routines aimed at the iliotibial band and surrounding muscle groups, like the quadriceps and hamstrings. These exercises can be incredibly beneficial, helping you regain function and alleviate discomfort.
As you progress, your physical therapist will likely recommend a gradual increase in your activity levels, typically no more than 10% per week. This careful approach minimizes the risk of overuse injuries, allowing you to rebuild your strength safely. For those who find themselves grappling with persistent symptoms, it is worth considering if manual therapy is appropriate, and additional interventions like corticosteroid injections or surgery may offer relief. At RegenCore, the treatment uses focused pressure waves to stimulate healing, enhancing blood flow and promoting collagen production. Many patients have shared their stories of significant improvements in mobility and pain reduction after this treatment, allowing them to return to the activities they love.
Creating a tailored treatment plan to your specific needs is essential for effective recovery, especially if you are wondering about long-term management strategies and for preventing future episodes. Physical therapists emphasize that a combination of focused exercises, adequate rest, and continuous evaluation can lead to successful outcomes in managing IT issues. With an incidence rate between 5% and 14%, it’s crucial to address this condition proactively. Professional guidance from physical therapists can help correct movement patterns and instill confidence in the effectiveness of your treatment. Moreover, integrating advanced therapies, including cell-based biologics, can further enhance your healing and recovery, paving the way for a brighter, pain-free future.
Conclusion
Understanding the connection between IT Band Syndrome and lower back pain is vital for athletes and active individuals. Many face the frustrating reality that a tight or dysfunctional iliotibial band can disrupt their biomechanics, leading to stress on the lumbar spine and significant discomfort. This awareness is crucial for effective management and recovery, allowing individuals to return to their beloved activities without the burden of ongoing pain.
Key insights reveal that IT Band Syndrome is particularly prevalent among runners and cyclists, underscoring the need for early identification and appropriate treatment. Factors like overuse, improper training techniques, and muscle imbalances can worsen this condition. It’s essential for athletes to embrace a holistic approach, incorporating strength training and proper warm-up routines into their regimen. Moreover, comprehensive treatment strategies, including physical therapy and regenerative therapies, can greatly enhance recovery and help prevent future complications.
Ultimately, addressing IT Band Syndrome not only alleviates knee pain but also plays a crucial role in preventing lower back issues. By raising awareness of the symptoms and implementing effective management strategies, individuals can take proactive steps toward maintaining their health and performance. Embracing a well-rounded approach to training and recovery empowers athletes to navigate the challenges posed by IT Band Syndrome, paving the way for a more fulfilling and pain-free active lifestyle.
Frequently Asked Questions
What is Iliotibial Band Syndrome (IT Band Syndrome)?
Iliotibial Band Syndrome is an overuse injury characterized by discomfort and inflammation along the iliotibial band, a band of tissue that stretches from the hip to the knee. It often results from repetitive friction of the IT band against the lateral femoral condyle during activities such as running, cycling, or hiking.
What are the common symptoms of IT Band Syndrome?
Common symptoms include sharp or burning pain on the outer side of the knee, particularly during activities like running or when sitting with bent knees. The pain can intensify with activity, especially during downhill running.
How prevalent is IT Band Syndrome among athletes?
IT Band Syndrome accounts for approximately 12.3% of running-related injuries, making it a common issue among athletes, particularly long-distance runners and cyclists.
What can exacerbate IT Band Syndrome?
Improper form or equipment can worsen IT Band Syndrome. Additionally, rapidly changing activity levels and inadequate warm-ups may also contribute to the onset of the condition.
What are the recommended management strategies for IT Band Syndrome?
Effective management often includes rest, physical therapy, and tailored rehabilitation exercises designed to strengthen the hip and improve flexibility.
How does RegenCore approach the treatment of IT Band Syndrome?
RegenCore offers personalized regenerative therapies using naturally derived cell-based biologics to promote healing and reverse tissue damage. Their approach is custom-tailored to support joint recovery and is backed by research demonstrating safety and efficacy.
Are foam rolling and massage effective for IT Band Syndrome?
Foam rolling and massage may not be effective for IT Band Syndrome due to the unique characteristics of the IT band.
Is there a connection between IT Band Syndrome and lower back pain?
Yes, recent studies indicate that there is a significant connection between IT Band Syndrome and lower back pain. About 30% of individuals with IT Band Syndrome may experience lower back pain due to tightness or dysfunction of the IT band affecting biomechanics and placing stress on the lumbar spine.
How can RegenCore help with both IT Band Syndrome and lower back pain?
RegenCore develops comprehensive treatment strategies that address both conditions, utilizing innovative Platelet-Rich Plasma (PRP) injections and Bone Marrow Aspirate Concentrate (BMAC) treatments to promote healing and improve injuries affecting tendons, ligaments, and joints.
List of Sources
- Define IT Band Syndrome: Understanding the Condition
- trainingpeaks.com (https://trainingpeaks.com/coach-blog/troubleshooting-runner-it-band-syndrome)
- Preventing and treating iliotibial (IT) band syndrome: Tips for pain-free movement – Harvard Health (https://health.harvard.edu/exercise-and-fitness/preventing-and-treating-iliotibial-it-band-syndrome-tips-for-pain-free-movement)
- emedicine.medscape.com (https://emedicine.medscape.com/article/91129-overview)
- Ground-breaking New Treatment for Iliotibial Band Syndrome (https://rtmslondon.com/iliotibial-band-syndrome)
- Explore the Link: IT Band Syndrome and Lower Back Pain
- Knee Pain, Hip Pain, Back Pain, and Your IT Band (https://fit4lifetampa.com/knee-pain-hip-pain-back-pain-and-your-it-band-understanding-the-connection)
- emedicine.medscape.com (https://emedicine.medscape.com/article/91129-overview)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC4458926)
- Can IT Band Cause Lower Back Pain? Understanding the Connection | RegenCore Method (https://regencoremethod.com/can-it-band-cause-lower-back-pain-understanding-the-connection)
- Identify Causes: Factors Leading to IT Band Syndrome
- trainingpeaks.com (https://trainingpeaks.com/coach-blog/troubleshooting-runner-it-band-syndrome)
- movementperfected.com (https://movementperfected.com/iliotibialband-syndrome-itbs-a-physiotherapy-case-study)
- The Iliotibial Band: A Complex Structure with Versatile Functions – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9023415)
- emedicine.medscape.com (https://emedicine.medscape.com/article/91129-overview)
- Proximal Iliotibial Band Syndrome in a Runner: A Case Report (https://onlinelibrary.wiley.com/doi/10.1016/j.pmrj.2018.06.017)
- Recognize Symptoms: Signs of IT Band Syndrome
- emedicine.medscape.com (https://emedicine.medscape.com/article/91129-overview)
- Dr Brandon Tauberg | Orthopaedc Surgeon | Sports Medicine Specialist Pittsburgh (https://brandontaubergmd.com/iliotibial-band-syndrome-orthopedic-sports-medicine-specialist-pittsburgh-pa)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC4458926)
- movementperfected.com (https://movementperfected.com/iliotibialband-syndrome-itbs-a-physiotherapy-case-study)
- IT Band Syndrome: Treating Knee Pain in Athletes – Marketplace Physical Therapy & Wellness Center (https://marketplacewellnesscenter.com/it-band-syndrome-treating-knee-pain-in-athletes)
- Discuss Treatment Options: Managing IT Band Syndrome
- Iliotibial Band Syndrome: Causes, Symptoms, and Treatment Options (https://opaortho.com/illiotibial-band-syndrome-itbs)
- movementperfected.com (https://movementperfected.com/iliotibialband-syndrome-itbs-a-physiotherapy-case-study)
- Preventing and treating iliotibial (IT) band syndrome: Tips for pain-free movement – Harvard Health (https://health.harvard.edu/exercise-and-fitness/preventing-and-treating-iliotibial-it-band-syndrome-tips-for-pain-free-movement)
- 30 Inspirational Physical Therapy Quotes – Care Options for Kids (https://careoptionsforkids.com/blog/physical-therapy-quotes)

