Introduction
Gluteal tendinopathy can be a challenging condition that significantly affects mobility and quality of life. Many individuals experience persistent hip pain that radiates down the thigh, making even the simplest movements feel overwhelming. This article explores the causes, treatment options, and recovery strategies for this increasingly common ailment, especially among older women and active individuals. As we deepen our understanding of gluteal tendinopathy, we’ll look at innovative therapies and rehabilitation techniques that can help alleviate discomfort and restore function, offering hope and support to those affected.
Define Gluteal Tendinopathy: Understanding the Condition
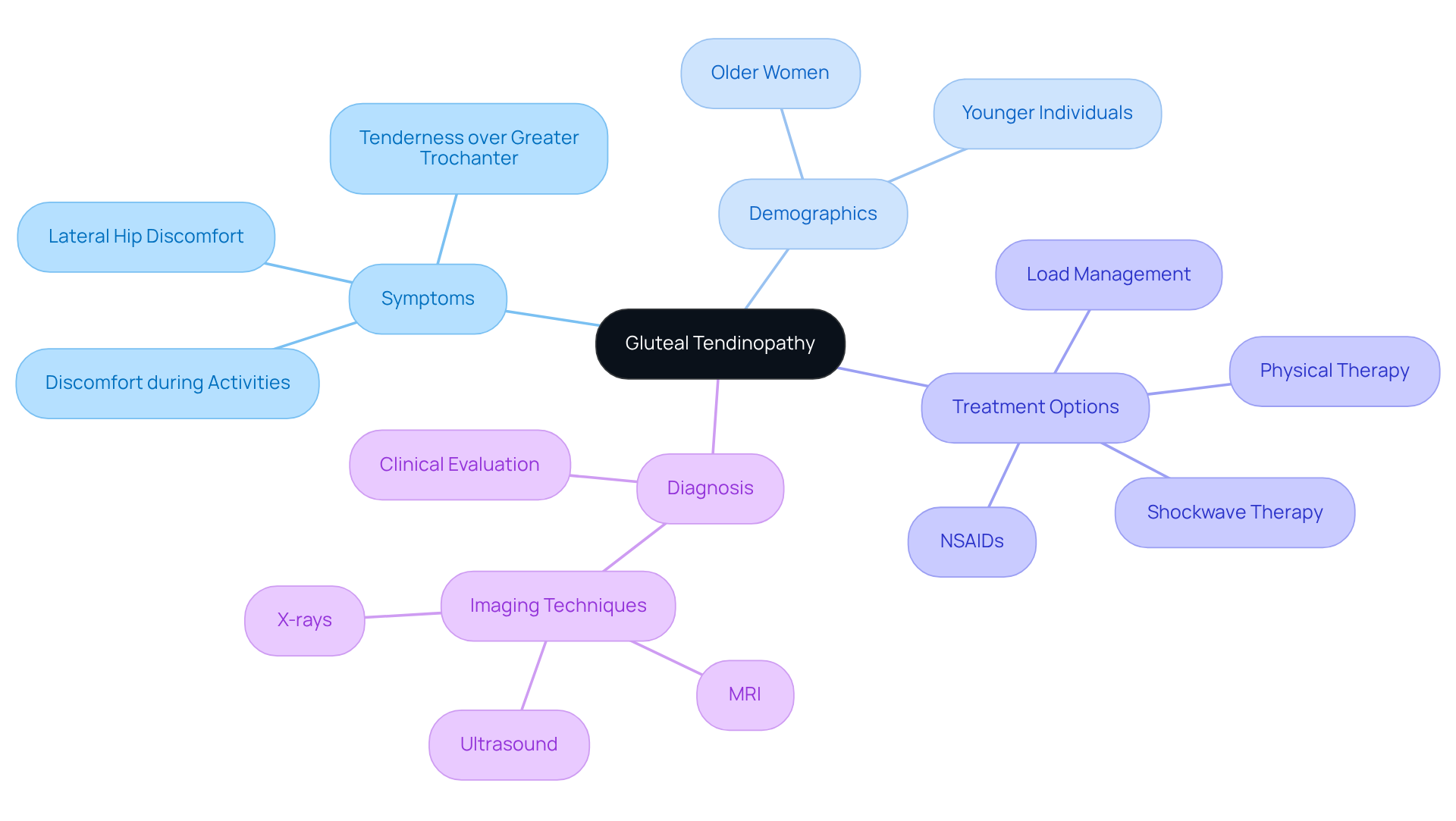
can feel like a heavy burden, marked by the degeneration or injury of the gluteal tendons, particularly affecting the gluteus medius and minimus muscles at the side of the hip. For many, this condition brings about persistent lateral hip discomfort that often radiates down the outer thigh, making everyday activities a struggle. Imagine the frustration of feeling tenderness over the greater trochanter, discomfort while walking or climbing stairs, and the unease of lying on the affected side. This discomfort can intensify with prolonged sitting or during weight-bearing activities, significantly diminishing the quality of life for those affected.
Understanding gluteal tendinopathy is vital for effective management. It’s especially common among older women, particularly those who have gone through menopause, yet it can also impact younger individuals who enjoy activities like running or dancing. While about 50% of those with this condition may find relief, many face considerable discomfort and functional limitations that call for intervention. Current research underscores the importance of a comprehensive treatment plan, which may encompass:
- physical therapy
- load management
- exercise modifications
- the use of NSAIDs
Recognizing and addressing symptoms early is crucial for recovery and preventing further injury, making it essential for anyone experiencing hip discomfort to seek a thorough assessment from healthcare providers.
At RegenCore, we believe in a compassionate, tailored approach to treatment. We incorporate innovative therapies that utilize naturally derived cell-based biologics, fostering healing and tissue restoration. These therapies can significantly benefit individuals grappling with gluteal tendinopathy. Research supports the effectiveness of such personalized regenerative treatments, often leading to improved function and pain relief within 8-12 weeks of structured therapy. Additionally, imaging examinations like MRI play a critical role in ensuring that each patient receives the care they truly need.
Identify Causes and Risk Factors of Gluteal Tendinopathy
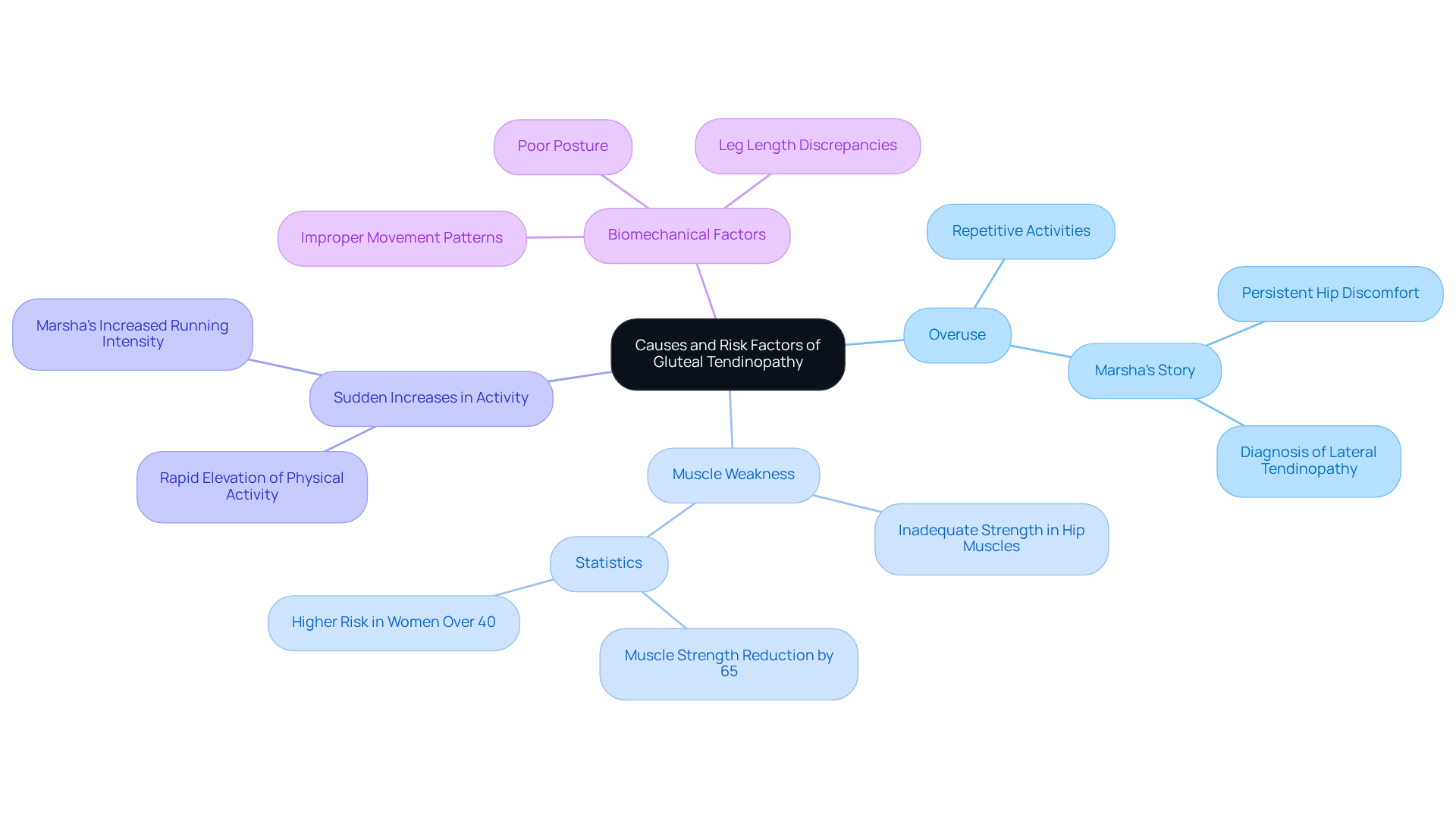
Multiple elements play a role in the progression of hip tendon issues, especially significant for active people. Key risk factors include:
- Overuse: Engaging in repetitive activities such as running, stair climbing, or prolonged sitting can place significant strain on the gluteal tendons, leading to injury. For example, Marsha, a passionate runner, experienced persistent hip discomfort from overuse, which was eventually identified as lateral tendinopathy.
- Muscle Weakness: Inadequate strength in the hip muscles can undermine hip stability, raising the chances of soft tissue injuries. This is especially prevalent in adults over 40, where muscle weakness is common. Statistics indicate that compared to the opposite side in individuals experiencing hip pain. Age and gender are important factors, as women, especially those over 40, face an increased risk for injuries due to hormonal changes and anatomical differences that influence connective tissue health. This demographic often experiences a decline in muscle mass, making them more susceptible to injuries.
- Sudden Increase: Quickly elevating physical activity levels without proper conditioning can strain the connective tissues, making them more vulnerable to injury. Marsha’s experience illustrates how a sudden increase in activity contributed to her condition.
- Biomechanical Factors: Issues such as poor posture, improper movement patterns, and leg length discrepancies can create abnormal stress on the tendons, further increasing the risk of tendon disorders.
Identifying these risk factors is crucial for individuals to take proactive steps in their physical activities, thus decreasing the chances of developing gluteal tendinopathy. At RegenCore, we offer innovative treatments such as physical therapy and regenerative medicine to enhance recovery and promote healing. These treatments specifically target the underlying issues associated with these risk factors, helping to restore strength and stability to the buttock area. As Jessie, another patient, noted, “I didn’t just get my hip back. I got my confidence back,” highlighting the importance of addressing these factors for effective recovery.
Explore Treatment Options: From Conservative Care to Regenerative Therapies
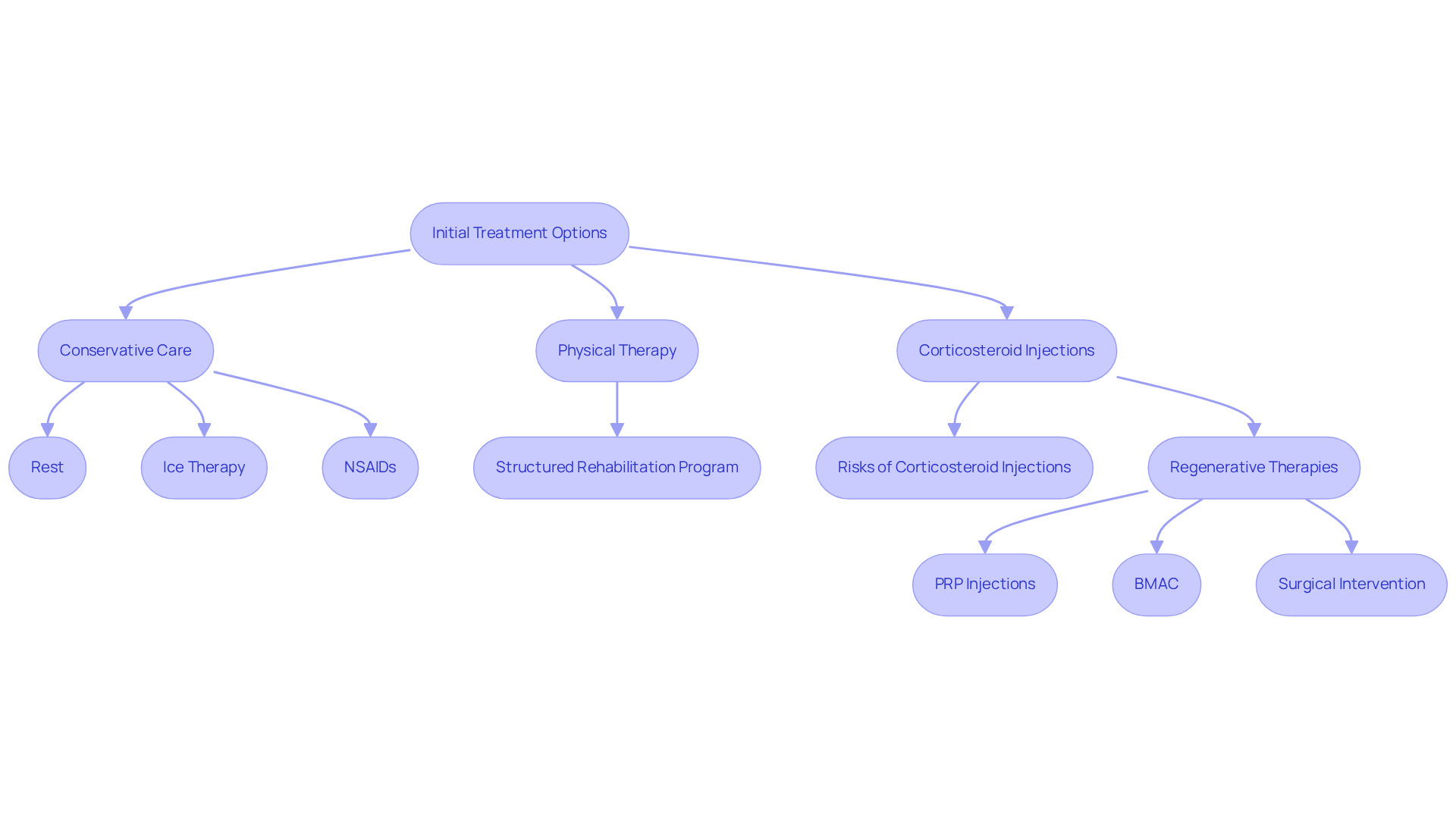
Dealing with gluteal tendinopathy can be a frustrating journey, filled with pain and uncertainty. Many patients find themselves grappling with discomfort that affects their daily lives, making even simple tasks feel daunting. The initial step in addressing this issue often involves conservative care. Rest, ice therapy, and non-steroidal anti-inflammatory drugs (NSAIDs) can provide some relief, but it’s important to be cautious. While these methods are effective for many, relying too heavily on NSAIDs can lead to complications like stomach problems and elevated blood pressure, adding to the stress of managing this condition.
As you navigate this path, rehabilitation emerges as a beacon of hope. A structured rehabilitation program can be transformative, focusing on strengthening the buttock muscles, enhancing flexibility, and correcting movement patterns. Research shows that patients who engage in rehabilitation often experience improved function and a reduction in discomfort. In fact, treatment success rates can soar to 90.9% at initial follow-ups, offering a sense of optimism for those seeking relief.
For those who continue to struggle with persistent pain, corticosteroid injections may provide a temporary respite. These injections can help reduce inflammation, but it’s essential to be aware of the risks, including the possibility of symptom recurrence and potential weakening of the connective tissue. This can be a tough decision, as patients weigh the benefits against the risks involved.
In recent years, regenerative therapies have gained attention for their potential to promote healing through the body’s natural growth factors. Options like platelet-rich plasma and stem cell therapy are increasingly recognized for their effectiveness. Research indicates that PRP therapies often yield superior results compared to traditional methods, especially for chronic cases. However, it’s crucial to understand that the efficiency of these treatments can vary based on the specific type of PRP used.
In critical cases where conservative treatments fall short, surgical intervention may be considered. While these procedures can provide relief, they come with longer recovery times and increased risks compared to non-surgical options. This can be a daunting prospect for many, but understanding all available treatments can empower patients to make informed decisions about their care.
By exploring these various treatment modalities, patients can find a path that resonates with their individual needs and circumstances. As advancements in treatment continue to evolve, there is hope on the horizon for those affected by gluteal tendinopathy.
Implement Rehabilitation and Long-Term Management Strategies
Recovering from gluteal tendinopathy can feel overwhelming, but implementing strategies are vital steps on your journey to healing. Let’s explore some key strategies that can help you regain your strength and confidence:
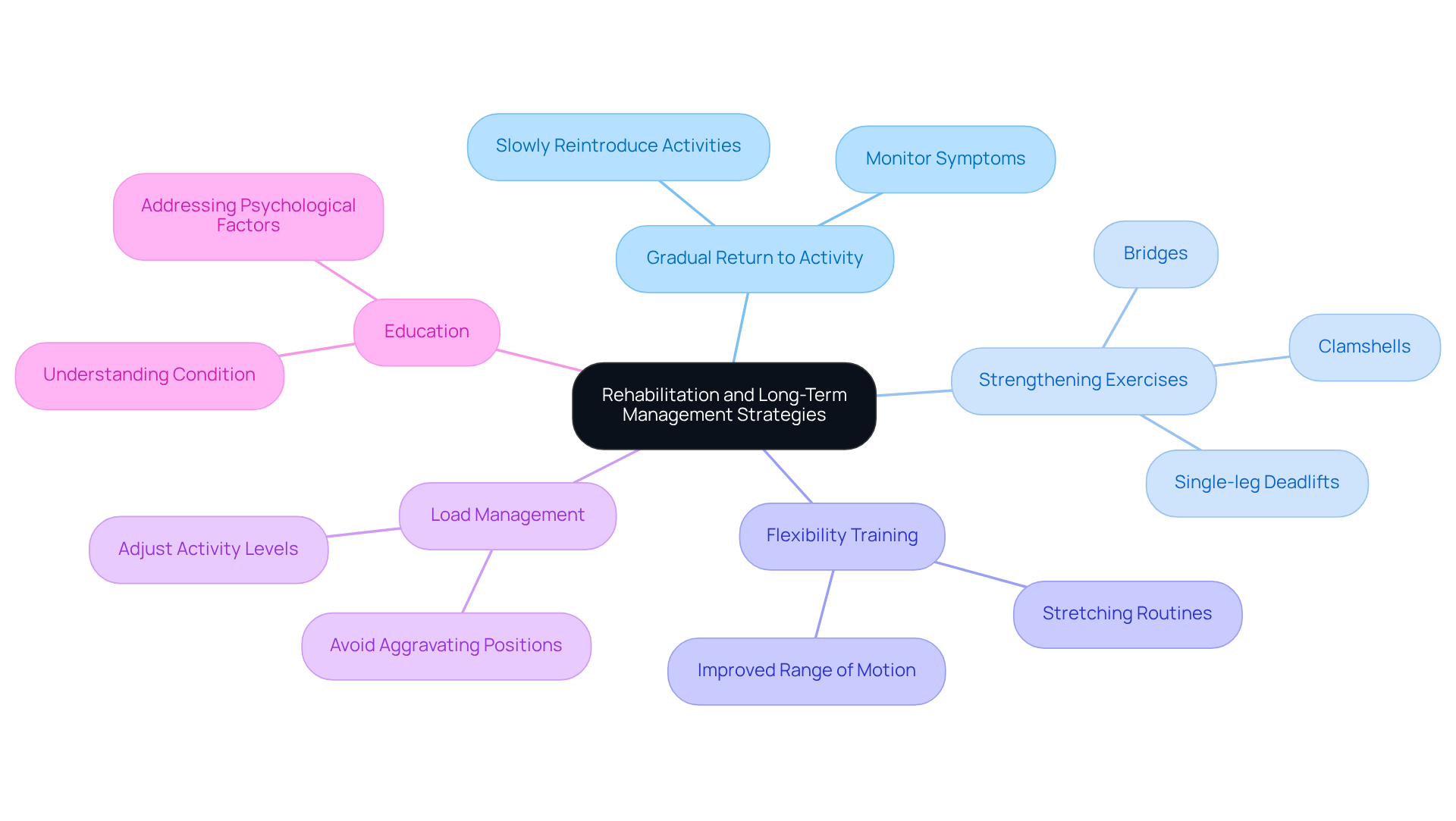
- Gradual Return to Activity: After the initial recovery phase, it’s important to slowly reintroduce activities while keeping an eye on your symptoms. This careful approach not only helps your recovery but also allows your body to adapt and strengthen its connective tissues over time.
- Targeted Exercises: Focusing on exercises that target your buttock muscles-like bridges, clamshells, and single-leg deadlifts-can significantly enhance your stability and support. These exercises are essential for maintaining hip function and preventing future injuries, including tendinopathy, giving you the tools to move freely again.
- Stretching Routines: Incorporating stretching routines for your hip and gluteal muscles can work wonders. Improved flexibility not only enhances your range of motion but also reduces tension on the tendons, making your movements smoother and more efficient.
- Activity Modification: It’s crucial to adjust your activity levels and steer clear of positions that might aggravate your symptoms, such as crossing your legs or sitting for long periods. Listening to your body during this phase is key to managing your symptoms and promoting healing.
- Education: Understanding gluteal tendinopathy and how to manage it empowers you to take an active role in your recovery. It’s also important to address any psychological factors, like fear of movement, as they play a significant role in your rehabilitation journey.
By embracing these strategies, you can pave the way for optimal recovery and enjoy long-term hip health. Remember, you’re not alone in this journey-support is available, and every step you take brings you closer to feeling like yourself again.
Conclusion
Gluteal tendinopathy can be a tough condition to navigate, especially for those who lead active lives or are facing the natural changes that come with age. It’s important to understand what causes this discomfort, recognize the symptoms, and explore the treatment options available. By prioritizing early intervention and personalized strategies, you can significantly enhance your quality of life and reclaim your mobility.
In this article, we’ve shared valuable insights into the risk factors that contribute to gluteal tendinopathy, such as:
- overuse
- muscle weakness
- biomechanical issues
We’ve also highlighted conservative treatments like:
- physical therapy
- load management
Along with innovative regenerative therapies, including:
- PRP injections
As effective pathways to recovery. Remember, a structured rehabilitation plan that gradually reintroduces activity, strengthens muscles, and improves flexibility is vital for your healing journey.
Ultimately, taking proactive steps to understand and manage gluteal tendinopathy is essential for your long-term health and well-being. Embracing a comprehensive approach that includes education, support, and tailored treatment can empower you to overcome the challenges this condition presents. If you’re experiencing symptoms, seeking professional guidance and exploring all available options can set you on the path to a successful recovery and a return to an active lifestyle.
Frequently Asked Questions
What is gluteal tendinopathy?
Gluteal tendinopathy is a condition characterized by the degeneration or injury of the gluteal tendons, particularly affecting the gluteus medius and minimus muscles at the side of the hip, leading to persistent lateral hip discomfort.
What are the common symptoms of gluteal tendinopathy?
Common symptoms include tenderness over the greater trochanter, discomfort while walking or climbing stairs, pain when lying on the affected side, and increased discomfort with prolonged sitting or during weight-bearing activities.
Who is most commonly affected by gluteal tendinopathy?
Gluteal tendinopathy is especially common among older women, particularly those who have gone through menopause, but it can also affect younger individuals who participate in activities such as running or dancing.
Can gluteal tendinopathy resolve without treatment?
Yes, about 50% of individuals with gluteal tendinopathy may find relief without treatment, although many experience significant discomfort and functional limitations that require intervention.
What are some treatment options for gluteal tendinopathy?
Treatment options may include physical therapy, load management, non-invasive therapies like shockwave therapy, and the use of NSAIDs (non-steroidal anti-inflammatory drugs).
Why is early recognition and treatment of gluteal tendinopathy important?
Early recognition and treatment are crucial for improving quality of life and preventing further injury, making it essential for individuals experiencing hip discomfort to seek a thorough assessment from healthcare providers.
What innovative therapies does RegenCore offer for gluteal tendinopathy?
RegenCore offers compassionate, tailored treatment approaches that incorporate innovative regenerative therapies utilizing naturally derived cell-based biologics, which promote healing and tissue restoration.
How effective are personalized regenerative treatments for gluteal tendinopathy?
Research supports the effectiveness of personalized regenerative treatments, often leading to improved function and pain relief within 8-12 weeks of structured therapy.
How are hip tendon issues diagnosed?
Imaging examinations like MRI or ultrasound play a critical role in accurately diagnosing hip tendon issues, ensuring that each patient receives the appropriate care they need.
List of Sources
- Define Gluteal Tendinopathy: Understanding the Condition
- goholistiq.com (https://goholistiq.com/gluteal-tendinopathy)
- Gluteal Tendinopathy: Symptoms, Causes & Treatment (https://my.clevelandclinic.org/health/diseases/22960-gluteal-tendinopathy)
- Gluteal Tendinopathy: Causes, Treatment, and Physiotherapy Solutions (https://keilorroadphysio.com.au/blog-articles/gluteal-tendinopathy)
- Managing Gluteal Tendinopathy.. What the Research Says Works Best! – Collins Avenue Physio (https://dublinphysiotherapy.com/managing-gluteal-tendinopathy-what-the-research-says-works-best)
- Identify Causes and Risk Factors of Gluteal Tendinopathy
- backinmotionsspt.com (https://backinmotionsspt.com/client-case-study-how-marsha-put-an-end-to-her-hip-pain)
- From Research To Practice: The Gluteal Tendinopathy Rehab Journey — Physio Network (https://physio-network.com/blog/gluteal-tendinopathy-rehab)
- Explore Treatment Options: From Conservative Care to Regenerative Therapies
- Pros and Cons of Using PRP for Tendon Injuries (https://sports-health.com/treatment/regenerative-medicine/pros-and-cons-using-prp-tendon-injuries)
- What Research Says About PRP for Tendons & Ligaments (https://avidsportsmed.com/what-research-says-about-prp-for-tendons-ligaments)
- Study: Platelet-Rich Plasma for Tendinopathy? Researchers See Promise (https://apta.org/news/2017/06/07/study-platelet-rich-plasma-for-tendinopathy-researchers-see-promise)
- mdpi.com (https://mdpi.com/2075-1729/14/12/1698)
- Implement Rehabilitation and Long-Term Management Strategies
- From Research To Practice: The Gluteal Tendinopathy Rehab Journey — Physio Network (https://physio-network.com/blog/gluteal-tendinopathy-rehab)
- running-physio.com (https://running-physio.com/gluteal-leap)
- exakthealth.com (https://exakthealth.com/en-US/blog/gluteal-tendinopathy-a-runner-s-guide-to-recovery-and-prevention)
- Effects of exercise-based interventions on gluteal tendinopathy. Systematic review with meta-analysis – Scientific Reports (https://nature.com/articles/s41598-024-53283-x)
- Managing Gluteal Tendinopathy.. What the Research Says Works Best! – Collins Avenue Physio (https://dublinphysiotherapy.com/managing-gluteal-tendinopathy-what-the-research-says-works-best)

